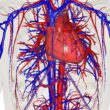
New 3-D printing technologies allow researchers to create patient-specific heart valve models that mimic the physiological qualities of the real valves. This image shows the submerged valve during flow testing. [Image from Rob Felt/Georgia Tech]
2. Heart valve replacements improve with 3D printed models
3D printed heart valve models are helping cardiologists prepare for valve replacement surgery.
Georgia Institute of Technology and Piedmont Heart Institute researchers are using standard medical imaging and 3D printing to make patient-specific heart valve models. The models are designed to replicate the physiological qualities of the real valves to improve the success rate of transcatheter aortic valve replacements by making sure a patient receives the right prosthetic and avoids paravalvular leakage.
“These 3D printed valves have the potential to make a huge impact on patient care going forward,” said Chuck Zhang, a professor at the Stewart School of Industrial and Systems Engineering at Georgia Tech, in a press release.
The 3D models allowed for doctors to test how prosthetic valves will interact with patient-specific hearts to predict leakage.
These models are created by a multi-material 3D printer that gives researchers control of design parameters to allow them to closely replicate the difficult anatomy of the heart.
“Previous methods of using 3-D printers and a single material to create human organ models were limited to the physiological properties of the material used,” Zhang said. “Our method of creating these models using metamaterial design and multi-material 3-D printing takes into account the mechanical behavior of the heart valves, mimicking the natural strain-stiffening behavior of soft tissues that comes from the interaction between elastin and collagen, two proteins found in heart valves.”
The researchers created the models using medical imaging of 18 patients who had valve replacement surgery. The heart models were then fitted with dozens of radiopaque beads to help measure tissue-mimicking material displacement.
Then, they paired the models with the same prosthetic that was implanted in the patient during their heart valve replacement surgery. They implanted the valves in a warm water testing environment that was made to simulate the inside of the body.
Software analyzed the location of the radiopaque beads before and after the prosthetics were implanted to determine how they interacted with the 3D models and if there were any leaks.