Pioneering simulation methods help researchers develop better devices.
Once considered risky, stent procedures today are viewed as safe and routine. In fact, every year more than one million patients with heart disease in the US receive stent implants. While stents save lives, side effects such as blood clots and heart attacks remain fairly common. Research in this area is complicated by the complexities of the human arterial system because there are too many variables and too much data to sift through.
Dr. Elazer R. Edelman, Professor of Health Sciences and Technology at Massachusetts Institute of Technology (MIT), Professor of Medicine at Harvard Medical School, and Dr. Vijava B. Kolachalama, postdoctoral associate at the Edelman Laboratory at MIT, are working to improve stents. Together, these researchers are helping to revolutionize the world of heart therapy using CFD modeling, bench-top experiments, animal modeling, and visualization.
Edelman and Kolachalama are using CFD to study how stents and drugs delivered from stents can treat arteries and simultaneously cause blood clots. They also hope to use the technology to predict whether specific arteries with stent implants are at risk of blood clots. “If we can accurately predict problems,” says Dr. Edelman, “we can help clinicians determine when to be more vigilant with patients about medications or additional procedures.” The results could help medical device companies develop safer, more effective stents and aid the in the regulatory approval process. Their work could lead to the ability to design individual stents for patients.
Today’s patient treatment
To reopen a blocked artery, physicians inflate a balloon at the end of a catheter inserted into the patient’s artery to compact atherosclerotic plaque against the artery walls. This proce-dure is known as angioplasty. Until recently, physicians would then install a small metal-mesh tube, or stent, to keep the plaque from snapping back into the artery. Stents prevent this recoil but tissue grows over the stent as part of a healing response. In 25-50% of cases, this reaction is so severe that flow through the artery is once again insufficient and another procedure is required.
To prevent the re-blocking, scientists started coating the stents with drugs, often imbedded in a thin polymer material for time release. Called “drug-eluting stents,” these implants have reduced the need for repeat procedures to less than 10%. Yet, even though the drug-eluting stents prevented tissue and plaque blockage, they created new and different issues for a small percentage of patients, resulting in life-threatening side effects such as blood clots and heart attacks.
Simulating complex results
Observing that the chance of blood clots rises along with the amount of drug delivered, Edelman and Kolachalama realized they needed an effective method for identifying and predicting drug delivery patterns from stents in complex arterial vessels.
Human trials and animal experiments provide valuable data related to the biologic response to stents and drugs. Yet, the researchers could not examine the issues of drug distribution variability from these studies alone. Modern imaging technology cannot provide a complete view of the drug patterns and patient variability made it impossible to track the large number of variables at play. Even subtle differences in the geometry of arteries or native disease, amount of drug delivered, change in drug absorption in different parts of the artery, or the way the stent is implanted can have dramatic effects in drug uptake.
Edelman and Kolachalama created physiologically relevant fluid dynamic models. The animal and human data served as right input conditions to the CFD models and the power of these tools was utilized by testing multiple variations in precisely the same manner repeatedly.
The goal was to simulate what would happen in an artery under multiple complex but physiologically relevant conditions. “It is precisely here that CFD modeling and visualization is ideal,” said Edelman. “We have helped people understand that CFD is a perfect tool for integrating physiologic data and complex non-intuitive conditions to answer important questions in medicine.”
The researchers began their work by gathering bio-metric data from several sources and in many formats to create mathematical models that would be solved against multiple variables or parameters. The simulation results, however, are in numerical format, making it difficult for the human brain to interpret. However, using the Tecplot 360 CFD visualization tool, Edelman and Kolachalama generated visuals that showed how the artery and drugs would behave under different conditions – similar to looking at the visual results from an X-ray or video scope.
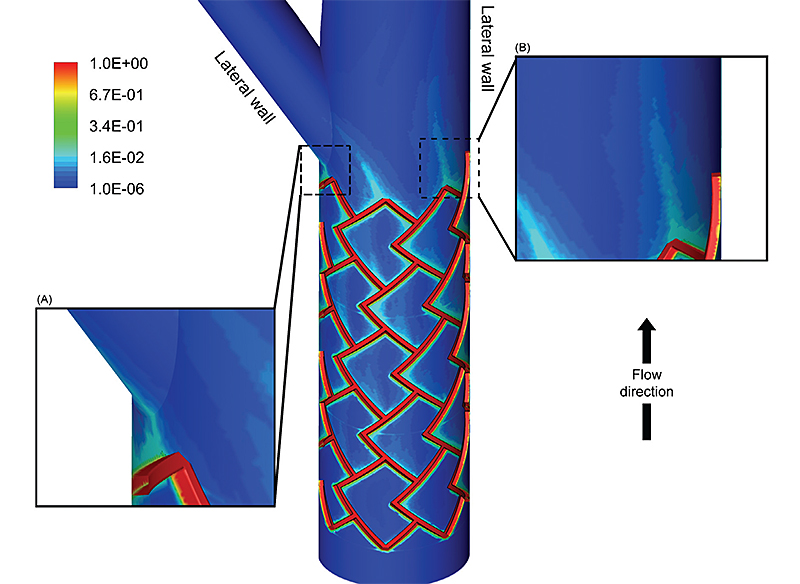
This image shows the surface contour map of drug concentration in a bifurcating artery. Drug is released from the surfaces of the stent where red color indicates regions of more drug. Blue indicates low drug concentration. The MIT researchers predicted that the complex pattern of the drug distribution depended on many factors including the blood flow that enters the bifurcation and the nature with which it splits at the fork. The insets show high magnification images of the drug pattern (B) on the lateral wall of the main branch and (A) near the region where the flow divides at the bifurcation.
The resulting images provided insight into how drugs deposited from a stent are affected by the positioning of the stent, changes in blood flow where arteries meet, and blood flow changes created by the stent itself.
“By observing the arterial drug distribution patterns for various settings, we understood that the drug released from the stent does not reach uniformly to all regions of the vessel; and this non-uniformity depends on where the stent is placed in the artery as well as the blood flow that is entering the vessel,” Edelman said. “Appreciating this phenomenon for more complex cases like branched vessels is non-intuitive, but we now have a computer model that gives us the much needed insight.”
Improving safety and effectiveness
The two researchers expect CFD modeling and visualization to improve both the safety and effectiveness of stent implants. “We now have the means to study stent placement in arteries in a manner not possible before,” said Edelman. “This has tremendous implications for engineers as they develop new devices designed to reduce the complications.”
In addition, Edelman and Kolachalama believe CFD modeling and visualization will help to streamline the regulatory process by providing the regulatory agencies the information they need to determine whether proposed changes to stent technology are significant enough to require a new clinical trial.
Ultimately, Edelman and Kolachalama expect CFD modeling and visualization will assist physicians in making better decisions for their patients. With different artery scenarios for each patient, scores of stent types and brands, and short timelines with which to make critical, life-saving decisions, doctors will be able to sort through data to select the best stent for a particular patient – based on fact rather than perception.
Tecplot CFD advantage
To obtain the advanced data visualization they needed, the researchers adopted Tecplot 360 CFD visualization software that lets you quickly plot and animate complex data with maximum precision, detail, and accuracy.
Tecplot helped the researchers use several different CFD pre-processing and solver packages, many of which are based on various formats. In addition, it’s been reported that Tecplot 360’s features are easier to use and faster to learn than other post-processors. And, image quality is very good, making it easier to hone in on the details within images. Similarly, the availability of “multi-block handling” allowed the researchers to turn certain blocks on and others off, thereby allowing them to select different parts of an artery and investigate just that area.
Edelman and Kolachalama believe CFD modeling and visualization will eventually allow doctors to use computers to compile all the options available, input them along with a patient’s medical data into a virtual artery, and sort through all the variables to determine which stent is best for that patient as they are doing the procedure.
MIT
www.mit.edu
Tecplot
www.tecplot.com
::Design World::




