The number of U.S. patients infected with a rare but dangerous fungal “superbug” called Candida auris has climbed quickly to 200 as of December 31, according to the latest figures from the federal Centers for Disease Control and Prevention.
In 2016, there were only seven cases of the multidrug-resistant infection on the national radar.
CDC first alerted American healthcare facilities that year to be on the lookout for the fungus, which can cause serious medical complications when it enters the bloodstream, usually through wounds, ventilators, or catheters. Patients with compromised health, especially those in hospitals and long-term care facilities, are most vulnerable.
“You won’t get it riding on the subway,” says Snigdha Vallabhaneni, a CDC epidemiologist.
Most of the cases, 123, have been reported in New York. New Jersey had the second-highest tally, 48. Other states reporting infections include California, Illinois, and Florida.
Candida refers to a wide variety of microorganisms in the yeast family, and some forms can live harmlessly in the body. About 20 varieties can cause infections — typically minor, such as athlete’s foot, nail fungus, oral thrush, and vaginal yeast infections. Candida auris raises concern because when it enters the bloodstream it can attack organs, Vallabhaneni says. Resistant to many medications, it is difficult to treat and can result in death.
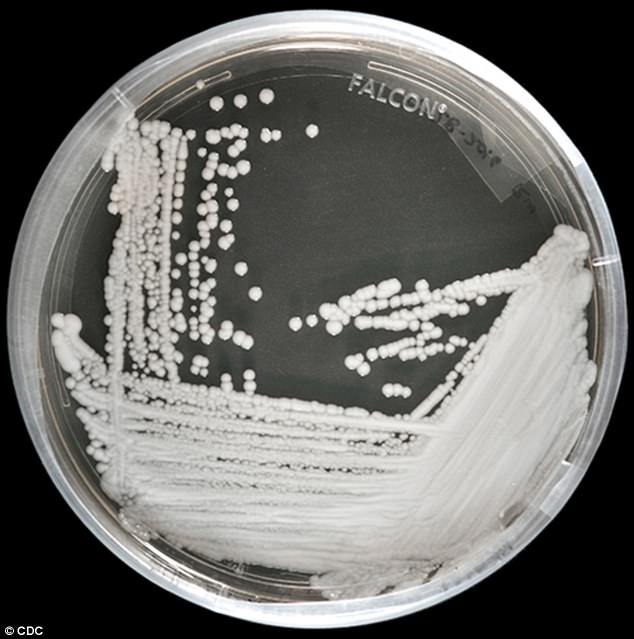
A strain of Candida auris cultured in a petri dish at CDC. (Image credit: CDC)
C. auris is transmitted easily between patients through contact with contaminated surfaces or person to person. It is often misidentified because it is difficult to recognize unless specialized technology is used.
C. auris “acts much more like a bacterial superbug” than other Candidaspecies, Vallabhaneni says.
About 40 percent of the U.S. patients who have contracted C. auris have died, according to CDC records. But since those patients had other serious medical conditions, it’s unclear how much of a role C. auris played in their deaths.
Many of the patients affected rely on medical equipment such as breathing tubes and central-line catheters that pump drugs into veins, offering an easy route for the fungus.
The CDC has begun prevention and education efforts targeted toward healthcare staff and the labs tasked with identifying C. auris. Much of the agency’s work has focused on improving labs’ abilities to identify the fungus, Vallabhaneni says.
Nancy Leveille, executive director of the Foundation for Quality Care at the New York State Health Facilities Association, said educational efforts by public health agencies such as the CDC and the New York State Department of Health have raised awareness. “There is attention,” she says, and that will help providers keep C. auris under control.
Anuradha Chowdhary, a professor and clinical microbiologist at the University of Delhi, was among the earliest scientists to identify the fungus in 2009.
She and colleagues recently published research showing that a certain mutation in the fungus’ genetic makeup may account for its widespread resistance to fluconazole, a common treatment for Candida infections. One promising treatment is a relatively new class of antifungal medications called echinocandins.
C. auris has been reported on five continents, in countries from the United States to Colombia to Britain. Yet the fungus’ origins aren’t easily explained.
Scientists can trace what may be C. auris’ earliest appearance to a 1996 South Korean case. But when they compare the genetic makeup of samples taken from regions around the world, they find the genes are different. It’s as if C. auris has sprouted up independently in each place.
When she first encountered it in Delhi, “I thought it was just our problem,” Chowdhary says. “I never imagined it would become so big.”
This story also ran on Kaiser Health News and Medill News Service.




