Rabies virus (RABV) transmitted by dogs is responsible for an estimated 60,000 human deaths per year, especially in Asia and Africa. If humans bitten by a rabid animal are treated quickly, the disease can usually be prevented.
Such post-exposure prophylaxis is expensive and should be reserved for bites from animals with confirmed infection, but testing dogs for rabies in resource-poor settings is challenging. A study published in PLOS NTD reports that six commercially available rapid rabies tests — which could make testing dogs much easier — fail to reproducibly yield accurate results.
The gold standard for rabies diagnosis is the fluorescence antibody test (FAT), which requires that brain tissue is fixed on microscope slides, stained with fluorescently labeled antibodies, and examined under a fluorescence microscope.
Alternative diagnostics include various assays to detect virus, antigen or viral RNA, the latter based on PCR technology. All of these tests require laboratory equipment, trained staff, and temperature-sensitive reagents.
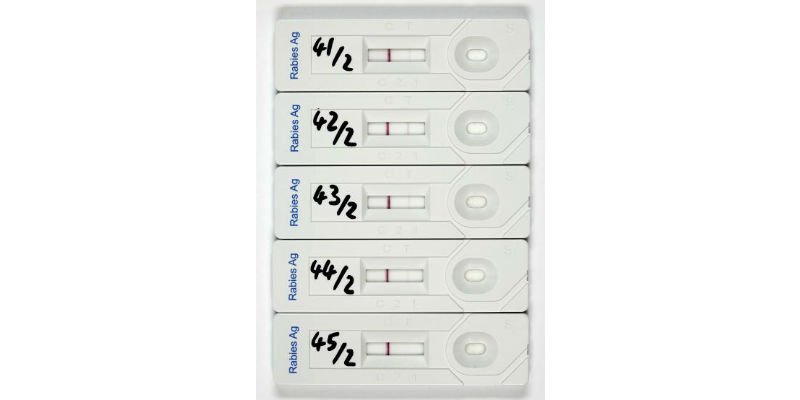
Results of five Rabies Antigen test strips. (Credit: Mandy Jörn)
In response to a call from WHO for better tests for the rapid and economical diagnosis of RABV, several alternatives have been developed.
Lateral flow devices (LFDs) have great potential as field tests: They are rapid and easy to use without the need for special training for implementation and evaluation, and can be shipped and stored at ambient temperatures. Early studies of rabies LFDs yielded promising results and raised hope for better rabies diagnostic capacity in resource-limited settings.
Following the initially reported prototype, numerous LFDs for rabies diagnosis are now commercially available. Because comprehensive evaluations of these tests have not been published, Conrad Freuling, from the Friedrich-Loeffler-Institute in Greifswald, Germany, and colleagues in this study compared six commercially available rabies LFDs.
They examined the sensitivity of the tests (their ability to exclude rabies infection accurately) as well as their specificity (reflecting an accurate positive diagnosis) in comparison with FAT and PCR in over 100 samples from experimentally infected animals and animals infected in the wild.
While all six tests showed good specificity (i.e., they did not come up with “false positives”), the researchers found that none of them demonstrated good sensitivity across the different sample sets.
In fact, more than half of all positive samples (i.e., those with positive FAT and PCR results) yielded “false negative” LFD results. Some LFD tests did better than others, and in some cases specific batches of the same test did better than others, but overall the results were disappointing.
On a positive note, the researchers report that viral RNA can be stored and eventually extracted from the LFDs using standard procedures available at molecular diagnostic laboratories. In fact, they were able to detect viral RNA after six weeks of storage at room temperature.
Thus test strips could be easily shipped by regular mail to a specialized laboratory, not only for a confirmation of the results, but also further characterization of virus isolates.
Discussing the results, the researchers say “with their current limitations commercially available rabies LFDs cannot be recommended for routine diagnosis and surveillance,” adding “If animals were involved in a biting incident to a human being, false negative results may induce the patient and the doctor to refrain from appropriate post-exposure prophylaxis (PEP) given its high cost, even if the leaflet accompanying the test states that results are to be confirmed by a reference method”.
They further conclude that “the observed limited sensitivity indicates a lack of quality control […] which should be the responsibility of the producers and not of the customers,” and emphasize that the study “is not meant to discredit the use of LFDs for rabies diagnosis but rather to encourage producers to substantially improve and assure the quality of their products.”




