Failure rates in some treatments using surgical mesh are unacceptably high according to a newly published comprehensive biomedical review that considers the findings from peer-reviewed scientific articles assessing its use. In addition, the review concludes that more experiments should have been conducted to properly assess how surgical mesh would behave in some of the bodily environments in which it has recently been used, such as the vagina and urinary system.
Surgical mesh is a fabric-like material which has been used, successfully, for over 50 years in the repair of hernias. In recent years, however, medical companies developed new products using this same mesh, for operations involving organs in the pelvic region. Many patients, the great majority being women, were implanted with pieces of mesh in operations to correct urinary incontinence and prolapse of organs such as the vagina, which frequently occurs after childbirth.
Many of these women have been condemned to a lifetime of pain and discomfort because the mesh has caused damage to surrounding organs and tissues, and it cannot be removed. As a result, the use of these products has been banned or restricted in many countries including the U.S., U.K., Australia, and New Zealand. In Ireland, medics and government have been slow to realize the extent of the problem, but in July this year the Minister for Health announced that a pause had been placed on the use of these products pending a full investigation into their use and the risks involved.
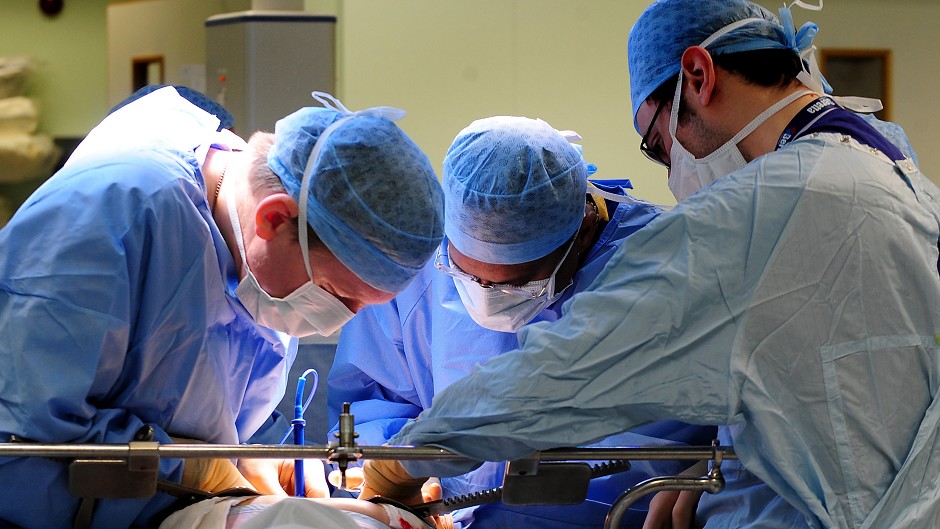
(Image credit: Associated Press)
The new review article, authored by David Taylor, professor of materials engineering at Trinity College Dublin, considers the findings of a wide variety of scientific and medical sources, from material test reports to clinical case studies. It has just been published by the Journal of the Mechanical Behaviour of Biomedical Materials.
“The use of surgical mesh to treat pelvic organ prolapse and urinary incontinence seems to provide another example in which new products have been developed that expand the use of existing materials without conducting the necessary experiments to properly understand the material, and how it will react in its new application,” says Taylor.
“Very severe consequences can result from mesh erosion, when the mesh material damages the surrounding tissues,” Taylor adds. “The prolapse products caused mesh erosion in over 10 percent of cases, rising to almost 30 percent in some studies, which I concluded was unacceptably high. In the case of urinary incontinence products, erosion occurs less often, around 2 percent to 3 percent, so my opinion is that patients should be given more information to allow them to make an informed decision about the risks involved. Chemical degradation of the material due to bacterial infection, and poor surgical technique are two potential reasons for the failures, but further work is needed – especially the examination of failed mesh products — to properly determine the underlying causes of this problem.”




