(Image by Allie Smith on Unsplash)
Hospitals across the U.S. have begun resorting to unorthodox means of replacing or sanitizing personal protective equipment (PPE) and atypical sourcing of PPE and other supplies needed to fight the coronavirus pandemic, according to a government survey.
The Department of Human Services’ Office of the Inspector General (OIG) conducted the random survey of 323 hospitals across 46 States, the District of Columbia and Puerto Rico during the week of March 23-27. Chief among their concerns was the continued shortage of PPE, which several reported was a result of the lack of COVID-19 tests and testing supplies and long waiting times for test results.
Having to wait seven days or more for test results caused hospitals to retain admitted patients who turned out not to have had the virus, causing staff to use up more PPE than might have been necessary and depleting other supplies such as drapes.
“Hospitals reported that widespread shortages of PPE put staff and patients at risk,” the OIG report said. “Hospitals reported that heavier use of PPE than normal was contributing to the shortage and that the lack of a robust supply chain was delaying or preventing them from restocking PPE needed to protect staff. Hospitals also expressed uncertainty about availability of PPE from federal and state sources and noted sharp increases in prices for PPE from some vendors.”
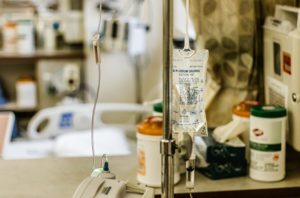
Other key hospital room supplies began running low, including IV poles, no-touch infrared thermometers, medical gas, linens, toilet paper, food, disinfectants and cleaning supplies, hospital officials said. Isolated and smaller hospitals reported facing special challenges maintaining and quickly restocking needed supplies.
Some hospitals reported turning to new, sometimes un-vetted and non-traditional sources of supplies and medical equipment such as online retailers, home-supply stores, paint stores, auto-body supply
shops and beauty salons, the survey said. This led to deliveries that came up short, were different from what was ordered, or contained items that were expired.
They also reported using ultraviolet sterilization of masks and having staff place surgical masks over N95 masks, bypassing sanitation procedures. Hospitals also reported turning to non-medical-grade PPE, such as construction masks or handmade masks and gowns, which they worried might put staff at risk. One hospital reported using 3D printing to manufacture masks, while another hospital reported that its staff had made 500 face shields out of office supplies.
“We are throwing all of our PPE best practices out the window,” one administrator told an OIG surveyor. “That one will come back and bite us. It will take a long time for people to get back to doing best practices.”
Fearing the growing ventilator shortage, hospitals began renting them, buying single-use, emergency transport ventilators or obtaining ventilators through an affiliated facility. Some hospitals reported converting other equipment, such as anesthesia machines, to use as ventilators. They also reported a scarcity of ventilator components such as tubes.
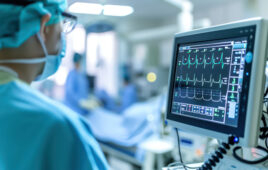
To keep the virus from spreading further, hospitals reported trying to screen everyone who entered, but the lack of no-touch infrared thermometers, which quickly measure a person’s temperature, caused long lines at hospital entrances. One hospital reported resorting to random screening while another said it could not take the temperatures of its 700-plus-member staff in a timely manner because it had just a few of the no-touch thermometers that could be devoted to staff testing rather than patient care.
A sales representative from a small Florida medical supplier told Medical Design & Outsourcing that the items in demand keep changing as the virus spreads and hospitals become busier. For example, last week they were seeking inexpensive IV poles, which cost about $50, but all that was left were higher-priced models, she said. In the past month, demand has periodically soared for other items, including masks, coveralls and thermometers, said the sales rep, who asked to remain anonymous.
“It’s a different product they’re looking for every week,” she said.