Lucile Packard Children’s Hospital Stanford has opened a new surgical center, marking a key milestone in the hospital’s expansion since it opened the doors of its new Main Building in December 2017. The Bonnie Uytensgu and Family Surgery and Intervention Center includes six new surgical suites and six interventional treatment rooms including radiology and cardiac catheterization labs, bringing the most advanced surgical, interventional and hybrid technologies available anywhere to Packard Children’s.
The hospital’s existing seven operating rooms (ORs) are currently undergoing upgrades and by early 2019, the hospital will have a total of 13 cutting-edge dedicated pediatric ORs — the most in any Northern California children’s hospital — nearly doubling Packard Children’s capacity for pediatric surgical procedures and enabling the hospital to perform an estimated 6,000 additional surgeries annually.
According to Surgeon-in-Chief James Dunn, MD, the new surgical center weaves powerful new imaging technologies into the operating suites, interventional radiology rooms, cardiac catheterization labs, and hybrid suites — improving real-time navigation as well as enabling the immediate evaluation of a procedure’s success, all of which serve to improve patient care.
The new surgery center is part of the greater Treatment Center at Packard Children’s, which also includes the state-of-the-art Cynthia Fry Gunn and John A. Gunn Imaging Center that opened in December 2017. With the new surgical suites open, the children’s hospital now has pediatrics-dedicated nuclear medicine, interventional radiology and surgical facilities all under one roof. This will also be the first time the children’s hospital will have pediatrics-dedicated cardiac catheterization (cath) labs, offering minimally invasive diagnostic and treatment techniques.
“Our Treatment Center brings an unprecedented collection of advanced technologies and procedural bandwidth to Packard Children’s,” says interim CEO, chief medical officer and pediatric general surgeon Dennis Lund, MD. “Creating the space and services specifically for children means they are spending less time under anesthesia and we are minimizing their exposure to radiation for treatments, which all translates to safer care, a better value and better experience for our patients and families.”
Before the new hospital opened, interventional radiology, nuclear medicine and surgical services were located in different parts of the hospital campus, and some services were shared with the adult hospital, Stanford Health Care. Now a patient can check into the Packard Children’s Treatment Center and go from service to service within one area without needing to be transferred between buildings, which improves patient safety.
Rebecca Claure, MD, medical director of Perioperative Services at Packard Children’s, explained that the Center’s condensed footprint facilitates better coordination of procedures, which reduces the number of times patients need to undergo anesthesia as well as decreases the length of time patients spend under anesthesia.
“Reducing the amount of time patients are under anesthesia also decreases their recovery time,” says Claure, who is also professor of anesthesiology at Stanford School of Medicine. “And removing the need to transport a patient over long distances is a big win for patient safety.” Claure noted that easier coordination of procedures also translates to fewer patient visits overall.
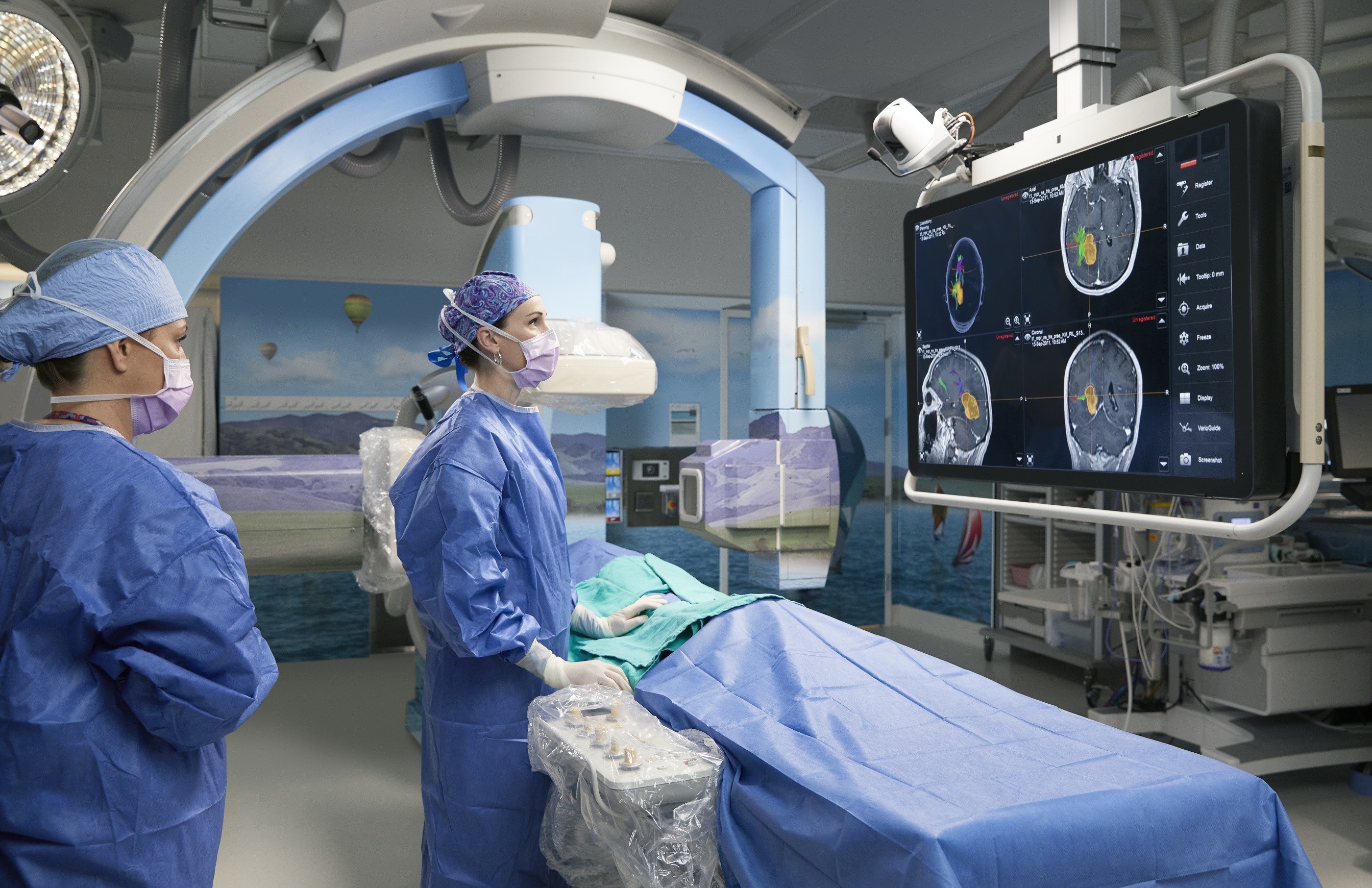
Neurosurgeon, Kelly Mahaney, MD, in the interventional neuroradiology (IR) room that is part of the neuro-hybrid suite, which allows care teams to perform a 3D intraoperative angiogram or an intraoperative MRI during surgery. (Image credit: Lucile Packard Children’s Hospital Stanford)
The new hybrid operating and interventional radiology suites have the greatest impact on center’s operational efficiency and capabilities, according to Dunn. A hybrid operating suite puts diagnostic imaging and interventional radiology services next door to an operating room, which allows multistage procedures that were previously performed in separate locations and at separate times to now be completed in one scheduled appointment time and location. The imaging technologies provide the lowest radiation doses available, and they also notify the care team if they are exposing an area to too much radiation. This is ideal for patients and everyone else in the room, including physicians, nurses and technicians.
In the neuro-hybrid suite, an intraoperative MRI (I-MRI) is positioned between an operating room (OR) and an interventional neuroradiology (IR) room that also doubles as an OR. Procedures that occur in the suite include removal of brain tumors, surgical treatment for epilepsy, and the surgical or endovascular management of neurovascular lesions in the brain such as Moya Moya disease, arteriovenous malformations (AVMs), or pediatric aneurysms. Traditionally, patients undergoing these procedures were moved from the operating room to the intensive care unit and then to MRI or angiography suite to determine whether a procedure was successful. Ready access to the highest quality 3 Tesla I-MRI during surgery now decreases the need for follow-up surgeries and lessens the amount of time the patient is under anesthesia, which shortens the patient’s recovery period and the overall time spent in the hospital.
The suite is the only of its kind dedicated to pediatric patients in Northern California and according to Gerald Grant, MD, chief of Pediatric Neurosurgery, it’s a huge advantage in providing the best care. “It’s very simply faster and safer for patients,” says Grant. “Being able to perform a 3D intraoperative angiogram or I-MRI is a game-changer. Immediately following a procedure, I am able to assure a family that we’ve successfully resected a tumor, for example.”
Packard Children’s is the first pediatric hospital in the world to implement the use of a robotic imaging technology suite called BrightMatter by Synaptive Medical Inc.
Traditionally, a disjointed collection of many data sources and tools have been used inside the OR, which required experts to manually piece together images and data to create a comprehensive view of the surgical field, Grant said. The new tool puts imaging, surgical planning, patient data collection, and intraoperative vision into a fully integrated platform with navigation, robotic automation, digital microscopy and data analytics.
“We now have unprecedented views of patient anatomy in 3D, which will allow surgeons to perform complex surgery on previously unreachably deep tumors of the brain with less invasive approaches and more precision,” says Grant. “Safer, less invasive procedures may lead to faster recovery times and fewer complications for patients and, in some cases, may render an inoperable diagnosis operable.”
In a dedicated cardiothoracic surgery suite, a new interactive virtual imaging platform will allow surgeons to view and manipulate layers of MRI and CT scans in an open 3-D space from inside the OR and without any special eyewear. This technology is the latest version of True3D, by EchoPixel, a Silicon Valley company. The technology was pioneered at Packard Children’s in 2017 and is rapidly evolving, according to Packard Children’s pediatric radiologist Frandics Chan, MD, who helped the company develop the technology. Chan expects that by the end of 2018, users will be able to link two True3D networks from anywhere in the world, opening the opportunity for real-time surgery consultations.
“This tool enhances our ability to understand each patient’s complex anatomy and better plan for surgery,” says cardiothoracic surgeon Frank Hanley, MD, chief of pediatric cardiac surgery at Packard Children’s. As one of the world’s leading experts on surgically correcting complex congenital heart defects, Hanley’s expertise is highly sought after by cardiac specialists throughout the country.
All of this new medical technology may be exciting for the care teams in the Treatment Center, but procedure rooms filled with overhead screens and giant machinery can be intimidating for children. Research has shown that keeping young patients as calm as possible before a procedure can improve clinical outcomes related to the induction of anesthesia and postsurgical recovery. To support that, many of the Treatment Center procedure rooms and machines are wrapped in whimsical scenes depicting nature landscapes.
Additionally, care teams in the Treatment Center are using a toolkit of immersive technologies aimed at reducing patients’ anxiety. For example, the CHARIOT (Childhood Anxiety Reduction through Innovation and Technology) Program at Packard Children’s uses virtual and augmented reality headsets to distract patients during minor procedures, blood draws, surgery prep and other potentially painful or stressful experiences in the hospital. Patients are responding positively to these interventions, and the CHARIOT team is actively researching the clinical impact of these technologies.
“Any time you have a child in the hospital, it can be stressful on the whole family,” says Lund. “In our new center, we are not only improving the quality and safety of treatments but also focusing on easing the experience for patients and families as much as possible.”




