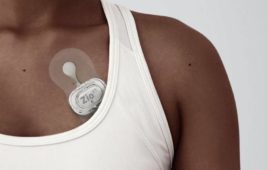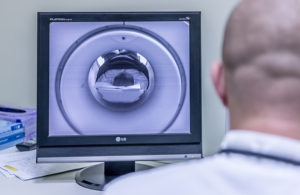
(Image by Michal Jarmoluk on Pixabay)
A medical imaging trade group today expressed concern about the CMS decision to further delay Medicare coverage for breakthrough devices.
The Medical Imaging & Technology Alliance (MITA) joined other medtech trade groups in voicing disappointment about the decision to delay the Medicare Coverage of Innovative Technology (MCIT) pathway until Dec. 15, 2021.
CMS issued a final rule on the MCIT in January, granting coverage for breakthrough devices the same day as their FDA approvals, for up to four years. Immediately upon taking office, the Biden administration asked federal agencies to consider delaying the effective date of rules published in the Federal Register to review questions of fact, law and policy the rules may raise. CMS officials decided that coverage of breakthrough devices warranted further review.
The MCIT rule was supposed to take effect on March 12, but CMS delayed it by another 60 days to give the public more opportunities to comment. Late last Friday, CMS came out with a decision delaying that coverage again until December.
The FDA grants breakthrough designation to certain devices that provide for more effective treatment or diagnosis of life-threatening or irreversibly debilitating diseases or conditions to get them to market faster.
MITA represents the manufacturers of medical imaging equipment, radiopharmaceuticals, contrast media and focused ultrasound therapeutic devices. The trade group is also concerned about updates to the definition of “reasonable and necessary” for purposes of CMS coverage.
The medtech industry and members of Congress had been pressuring CMS to enact the final rule. But physicians’ organizations and the insurance industry pushed back, citing safety and efficacy concerns for devices not thoroughly tested. The American Medical Association raised concern about the lack of opportunity for stakeholder review and input about these coverage decisions and about allowing private payor coverage policy to determine whether an item is “reasonable and necessary” for purposes of Medicare coverage.
“We are greatly disappointed by the CMS decision to postpone implementation of MCIT,” said MITA executive director Patrick Hope in a news release. “Once implemented, MCIT will modernize Medicare’s current reimbursement structure, ensuring broader beneficiary access to Food and Drug Administration (FDA)-authorized, breakthrough medical technologies that would otherwise be unavailable. Further delaying this coverage pathway effectively denies patient access to breakthrough technologies and ‘kicks the can down the road,’ leaving patients, healthcare providers, and medical device innovators in limbo.”
The delay also sparked concern among other medtech trade groups, including AdvaMed and the Medical Device Manufacturers Association. The new delay allows for further review from interested parties.
“Despite our concerns, we will continue our engagement with the agency to support the implementation of MCIT before the end of 2021,” Hope said.