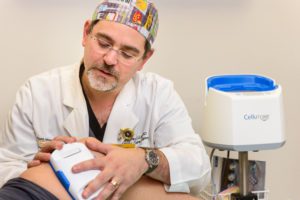
Dr. Jeffery Litt is a burn and wound care physician at University Hospital. The Acelity graft harvesting device eliminates the need for doctors to handle skin grafts with their hands. [Photo courtesy Missouri University]
The researchers used the Acelity Cellutome Epidermal Harvesting System. It is an automated, precise and reproducible process that offers minimal pain and less donor-site trauma. It features suction microsomes that harvest epidermal micrografts automatically, eliminating the need for physicians to handle grafts.
“Chronic wounds occur when healing fails to progress normally and persists for more than 30 days,” said Dr. Jeffrey Litt, assistant professor of surgery at the Missouri University (MU) and lead author on the study. “Current treatments such as moist dressings, frequent irrigations and wound cleaning are not always enough to ensure that healing occurs in high-risk patients. Although a skin graft can be used to close a wound that refuses to heal, the surgical technique usually is painful, time-consuming and leaves significant donor site wounds.”
Chronic wounds affect about 6.5 million Americans. They account for diabetic ulcers, pressure sores, surgical site wounds and traumatic injuries to high-risk patients. It costs the U.S. around $25 billion annually to treat chronic wounds, according to the National Institutes of Health.
One of the most common methods for treating traumatic and burn injury-related skin loss is split-thickness skin grafting. This procedure removes the top two layers of skin from a healthy donor and transplants the tissue to the injured skin. This method has to be done in an operating room and is reliant on donor skin.
The MU Health Care study involved 13 patients with different types of chronic wounds. The autograft harvesting system technology only harvested the top layer of the skin for a more consistently sized donor graft. The results showed less damage to the donor site and offered little to no pain for the person receiving the skin graft. This approach, being minimally-invasive, can also be done from an outpatient clinic. Those who received the skin graft showed no wound reoccurrence after the procedure.
“Eight of the 13 high-risk patients treated with the autograft system experienced much faster healing of their chronic wounds,” Litt said. “Four of these patients fully healed in less than one month. Additionally, the comparatively rapid closure of the open wounds also reduced health care costs by an average of $1,153 per patient and $650 to the burn and wound program.”
The study was published in the Cureus Journal of Medical Science.
[Want to stay more on top of MDO content? Subscribe to our weekly e-newsletter.]




