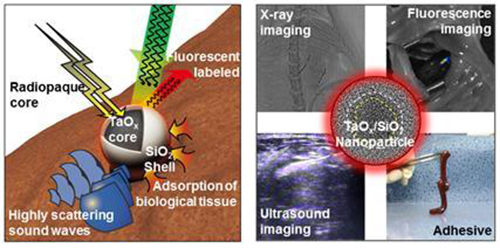
Nanoparticles made with a shell of silica (SiO2) and a core of radiopaque tantalum oxide (TaOx) are used to make a tissue adhesive and visible to ultrasound, X-ray, and fluorescent imaging. (CREDIT: IBS)
As open surgery has gradually been replaced by minimally-invasive and image-guided procedures, tissue adhesives are taking the place of sutures and surgical staples. With countless applications, including: bleeding embolization, angioplasty, stent insertion, and biopsy, among others, new surgical glues are highly desired in medical clinics. Researchers at the Center for Nanoparticle Research, within the Institute for Basic Science (IBS) in collaboration with medical doctors in Seoul National University Hospital, created a surgical glue that is both adherent and visible in the most common imaging techniques: fluoroscopy, ultrasound, and computed tomography (CT). It is the first nanoparticle-based tissue adhesive that features these characteristics. Its properties were successfully tested in sealing a liver puncture and in conducting operations in moving organs, like lung and limbs. The full results of these surgical procedures conducted in animal models are available on Nature Communications.
IBS scientists in collaborations with researchers led by Nohyun Lee (Kookmin University), Hyo-Cheol Kim (Seoul National University Hospital) designed nanoparticles with a shell made of silica (SiO2) and a core of radiopaque tantalum oxide (TaOx). SiO2 holds the tissue together, while TaOx provides contrast enhancement on ultrasound and CT.
The research team tested the TaOx/SiO2 core/shell nanoparticle (TSN) glue and found that it is clearly visualized by real-time imaging modalities and exhibits adhesive properties similar to that of the U.S. Food and Drug Administration (FDA)-approved cyanoacrylate and Lipiodol (CA-Lp), a mixture of a tissue adhesive and radiopaque oil used in the clinical practice.
Its stickiness, due to the absorption of the silica surface to the tissues, was tested to suture a puncture in the liver of a rabbit in a minimally invasive procedure, without abdominal incision. “A plethora of surgical procedures create a liver puncture, which necessitates hemostasis to stop the bleeding. These include operations frequently used in patients with chronic liver disease and liver cancer, such as: liver biopsy, percutaneous biliary drainage, portal vein embolization, and portal vein angioplasty,” points out SHIN Kwangsoo, the first author of this study.
Beyond adhesiveness properties, TSN is more biocompatible than CA-Lp, meaning that it causes less side effects. CA-Lp tends to trigger immune reaction within three days from the operation and inflammation after 14-65 days, while experiments showed that TSN did not show such adverse effects after 56 days.
TSNs also ensured accurate target localization during movement; when TSNs were injected in rat’s thigh and calf muscles, they did not move even during the flexion and extension of the leg. “TSNs are well fixed to tissues so that nanoparticles and tissues move in unison. This is important because they could help surgeons to recognize a moving surgical target and perform a safe and accurate operation,” explains HYEON Taeghwan, director of the IBS Center for Nanoparticle Research.
Finally, IBS scientists verified that TSN is stable in one of the most moving organs; the lungs. A fluorescent version of TSN visible under CT was successfully used to guide the resection of lung cancer in a rat. The opacity of TSNs was high enough to be clearly distinguished from the nearby ribs and vertebrae.




