Using a combination of DNA sequencing and computer science techniques, a team of researchers has developed a new method for monitoring the health of organ transplant patients — one that promises to provide life-saving clues to diagnose organ rejection at an early stage.
More than 180,000 people live with organ transplants in the U.S., and many undergo costly and risky biopsies to determine if their body is accepting or rejecting an organ. An alternate method demonstrated by Iwijn De Vlaminck, who is also a senior author of the current study, found that cell-free DNA (cfDNA), essentially fragments of dead cells derived from an organ, can be detected in a patient’s bloodstream and used as a proxy for the organ’s health. The more cfDNA that is discovered, the greater the likelihood the organ is failing. But without knowing the donor’s DNA — which is often the case — doctors have no reference to identify the cfDNA.
But now a research team from Cornell and Stanford University has demonstrated a method for identifying cfDNA without the donor. To address the issue, Eilon Sharon, postdoctoral researcher with Jonathan Pritchard, and colleagues worked to develop a computer algorithm that estimates the donor-derived cfDNA and can predict heart and lung rejection with an accuracy similar to that in cases where donor information is available. Their work, published in open-access journal PLOS Computational Biology, also details a refined algorithm to address closely related recipients and donors, a scenario that is common in bone marrow and kidney transplantations.
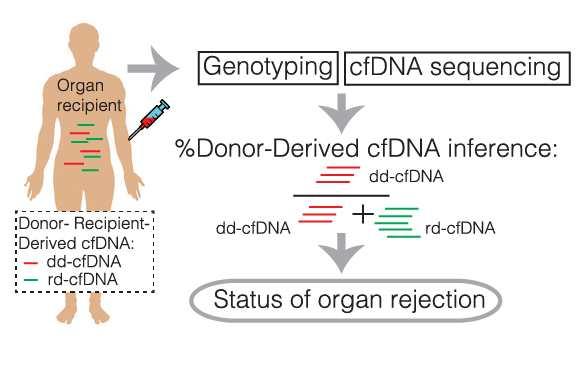
(Image credit: Sharon E, Shi H, Kharbanda S, Koh W, Martin LR, Khush KK, et al)
The algorithm uses publicly available genotypes and techniques of relationship inference to model which cfDNA fragments are most likely from the organ.
“Specifically, the model infers the donor’s most probable ancestral population and accounts for close relationship by detecting DNA segments that are identical due to close descent,” says Sharon, adding that the phenomenon is known as “identity by descent.”
The findings alleviate a major barrier to using cfDNA detection — also known as genome transplant dynamics — instead of biopsies, and researchers hope the computer science-based method will help save lives. Accurate monitoring of organ health is essential to a patient’s long-term survival; currently, the median life expectancy for a heart transplant patient is around 11 years, and only 5.3 years for recipients of lungs.
“We are excited about the multiple applications for this method in transplantation medicine and we are looking forward to seeing it used in clinical settings,” says De Vlaminck.




