Previous studies about nurse workflow have used time-motion study methods, which involve manually observing nurses in person or on video and then clocking how much time they spend on each task. Now, a University of Missouri engineer has developed a method for better tracking how nurses in an intensive care unit (ICU) spend their workday. The method uses a combination of manual observation and non-intrusive tracking sensors that allow researchers to track nurses in real time. Findings could help improve the health care delivery process in the ICU and could also be applied to other health care procedures.
“The nurses in an ICU confront heavy daily workloads and face difficulties in managing multiple stressors from their routine work,” says Jung Hyup Kim, an assistant professor in the MU Industrial and Manufacturing Systems Engineering Department. “They’re multitaskers, doing many things simultaneously. For example, while talking with the patient and getting vital signs, they also are charting in the electronic medical record (EMR) system. We wanted to find ways to streamline their jobs, making them more efficient.”
Kim uses a Near Field Electromagnetic Ranging (NFER) system to drill down to a more accurate measure of how much time ICU nurses spend on various duties each day. The NFER system, which includes several routers set up throughout the unit that track devices worn by the nurses, allows researchers to track nurses’ movements in real time. These movements and workflows are observed on monitors showing dots that represent health care workers as they move about and perform their duties.
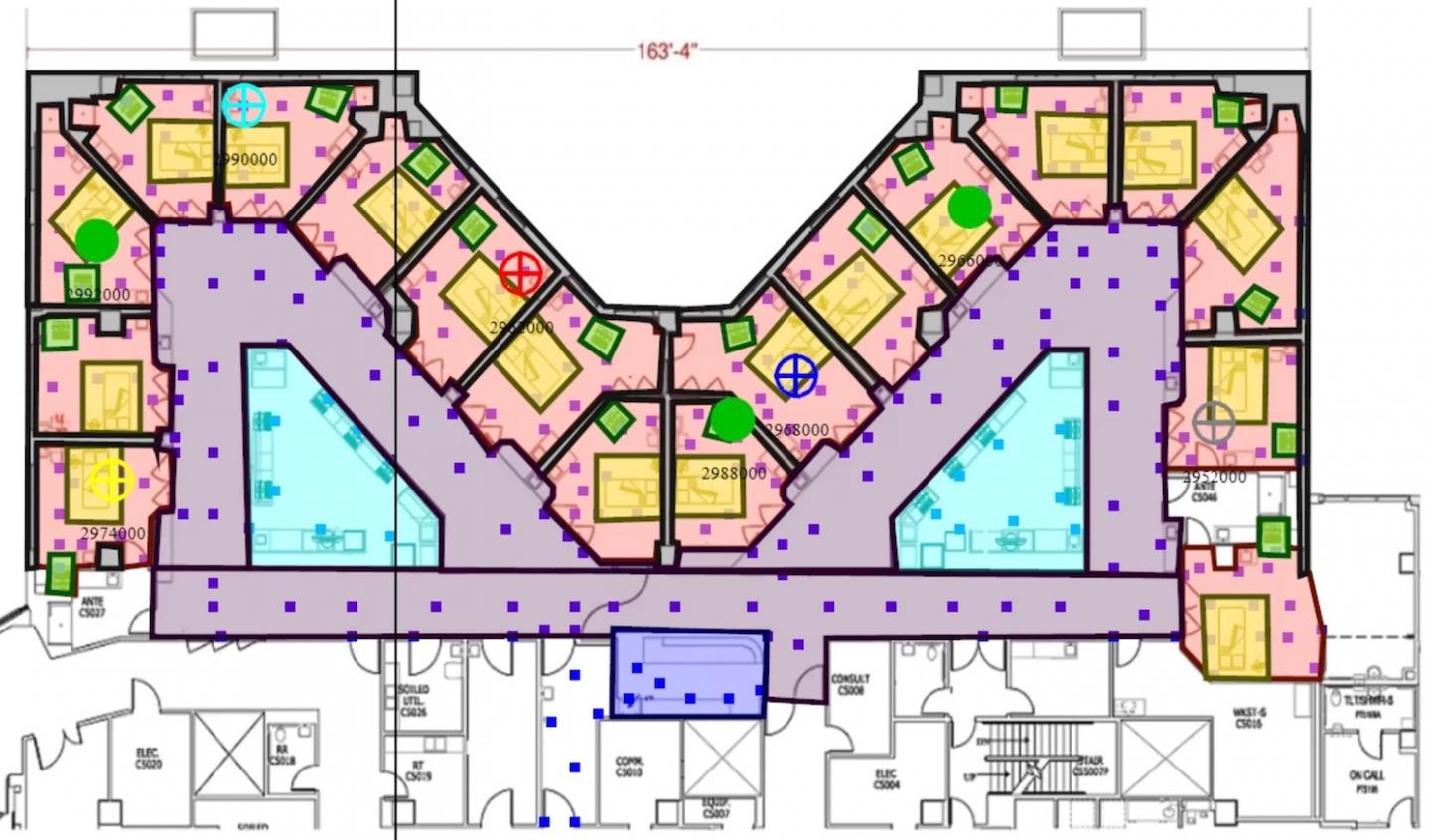
The NFER system, which includes several routers set up throughout the unit and wearable devices for the nurses, allows researchers to track nurses’ movements in real time. (Image credit: Jung Hyup Kim)
Researchers often are not allowed to accompany nurses into patient rooms in order to protect patients’ privacy. The NFER system allows researchers to observe if nurses are providing patient care or inputting data during their time spent in each room. Using the tracking system, Kim and his team were able to pinpoint whether nurses were at the room’s computer or bedside and measure time spent doing each accordingly.
“We knew when and where nurses were during their shift and what kind of work they did in real time by using the data we collected from the NFER system. I believe it will advance our understanding of ICU nurses’ workflow,” Kim says. “Future planned studies will cover full 24-hour periods rather than just the day shift, as well as extend the method to other ICUs.”
Using these measurements, managers and supervisors can help plan nurses’ shifts more efficiently, and designers and architects can use the information to design more efficient hospital units, Kim says.




