According to clinical studies, about a third of patients with atrial fibrillation will suffer a stroke during their lifetime. Between 70 and 90% of these strokes are caused by a thrombus formed in the left atrial appendage.
In patients with contraindications to oral anticoagulants, a left atrial appendage occluder (LAAO) is often implanted to prevent blood flow entering in the LAA. But this strategy is not without problems and often the success of the device depends on the clinician’s experience. Implementation can even lead to blood clots outside the device, eventually leading to stroke if not treated.
The aim of a study, published in March in Frontiers in Physiology, was to develop tools based on biophysical models and interactive interfaces to optimize LAAO device therapies. The study was led by Òscar Camara, a researcher with the Physense Research Group, which is a part of the BCN MedTech Unit at the UPF Department of Information and Communication Technologies (DTIC). “A study that summarizes the good work of our research team over the past three years and is part of the bachelor’s degree final project in Biomedical Engineering by Ainhoa M. Aguado, first author of the study”, explains Camara.
VIDAA, a web-based 3D interactive virtual implantation platform
To obtain the most appropriate LAAO configurations for a given patient-specific LAA morphology, the researchers created a web-based 3D interactive virtual implantation platform called VIDAA. Then, based on the features of the shape of the patient’s appendage, the researchers calculated the most promising LAAO device.
Using the geometric and anatomic data of the patient’s left atrial appendage, together with the most suitable ad hoc device, volumetric meshes were built to run computational fluid dynamics simulations. Thus the researchers were able to assess estimated blood flow patterns after device implantation.
Thus, by combining the VIDAA platform with computational simulations it has been possible to identify the LAAO configurations associated to a lower risk of thrombus formation and also to reveal that the positioning of the device is a key element in the creation of regions with turbulent blood flows after implantation.
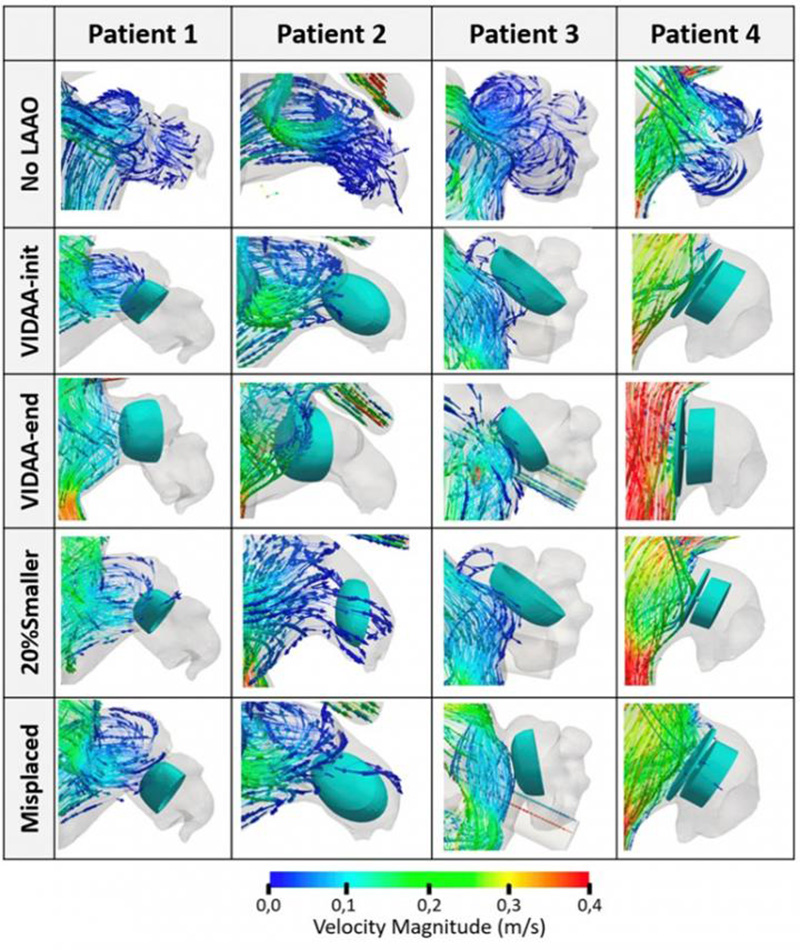
Blood flow streamlines in the left atrial appendage (LAA) from haemodynamics simulations of the four patients under study. Credit: UPF




