For patients undergoing weight loss (bariatric) surgery, losing at least 8 percent of excess weight just one month before the procedure directly impacts their ability to shed even more pounds in the year following surgery, according to new study findings published as an “article in press” on the website of the Journal of the American College of Surgeonsahead of print.
Apart from the weight-loss procedure itself, diet and weight loss before the operation may also determine how successful a person is in losing pounds during the first year after the procedure.
“Currently, controversy exists for the optimal preoperative dietary optimization of patients prior to bariatric surgery. On one side, insurance policies often mandate six or 12 month weight management programs. This mandate is in direct contrast to many bariatric surgeons, who prefer to use short-term, calorie-restricted diets several weeks prior to surgery in order to optimize outcomes,” says study coauthor John David Scott, MD, FACS, FASMBS, associate professor of surgery, University of South Carolina School of Medicine, Greenville, and the metabolic and bariatric surgery director of Greenville Health System (GHS), South Carolina.
Led by Deborah A. Hutcheon, DCN, RD, LD, clinical nutrition specialist at GHS, the study looked specifically at the role of a short-term, surgeon-recommended preoperative diet in improving patient outcomes, such as weight loss, following surgery. The study involved 355 patients who undertook the recommended four-week low-calorie diet before undergoing a bariatric operation, either sleeve gastrectomy or Roux-en-Y gastric bypass, between January 2014 and January 2016 at GHS.
“Our ultimate goal was to see what makes postoperative outcomes better for our patients undergoing this lifesaving procedure,” Scott says.
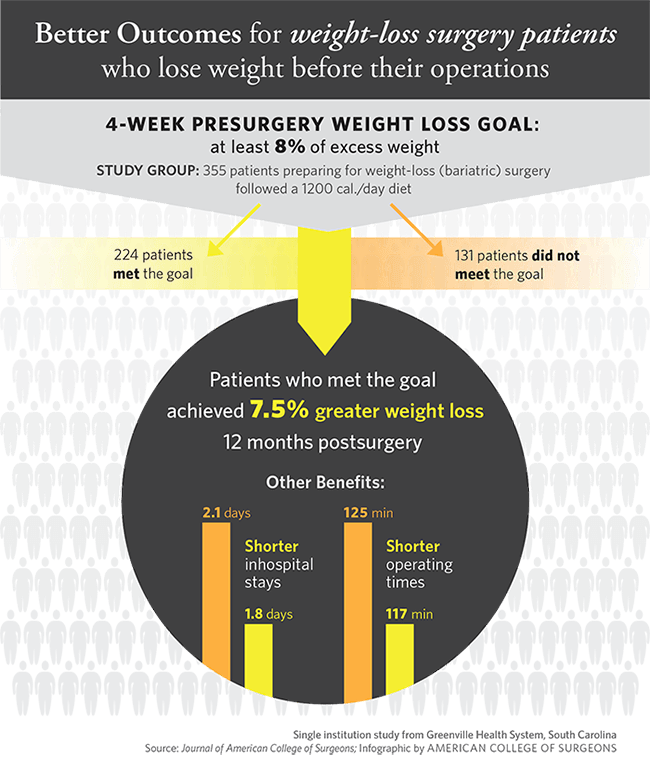
Patients who lose some excess weight prior to weight loss surgery achieve greater weight loss after surgery, and also experience shorter hospital stays and shorter procedures. (Image credit: American College of Surgeons)
The study patients were asked to lose at least 8 percent of their excess weight by following a 1200 calorie diet for four weeks immediately preceding their operations. For the analysis, the patients were divided into two groups based on whether they actually achieved that weight loss goal (224 patients achieved that goal, and 131 did not).
Patients who lost at least 8 percent of their excess weight achieved a 7.5 percent greater weight loss at the 12-month post-surgery mark, compared with those who did not achieve that weight loss goal. This finding held true even when other factors such as age, gender, ethnicity, and health problems including high blood pressure and diabetes were considered.
Hutcheon explains that there is this key window of opportunity after bariatric surgery, up to 18 months, when many physical and metabolic changes occur that help facilitate weight loss. “After that time point, patients will have to rely on diet and exercise and lifestyle management to maintain that weight loss,” she says.
“We call it the honeymoon period of bariatric surgery,” Scott adds. “After a year or year and a half, your body starts to figure out what it can and can’t do, and your behaviors may change a little bit, so the odds that you are going to lose a significant amount of weight after that time period are definitely decreased. Therefore, the more weight you can lose during that honeymoon period, the better, because that effort will help establish a set point, in terms of where your steady weight is going to be further down the road.”
The analysis also showed a reduction in hospital length of stay (1.8 days vs. 2.1 days) for patients who achieved that target weight loss (8 percent or greater), and the average operative time was shorter (117 minutes vs. 125 minutes) for that group as well.
“Ultimately, we believe that preoperative preparation for bariatric surgery should be mediated by individual surgeons taking care of their patients,” Scott says. “And this 8 percent target should not be used as a hard set point to qualify patients for bariatric surgery. Because patients with obesity who weren’t able to achieve that 8 percent goal still had dramatic effects in terms of how much weight they lost and comorbidity resolutions.”
The most important aspect of this study is that it adds to the body of research data showing that it is beneficial for bariatric surgery programs to encourage and counsel patients to follow a short-term diet or aim to achieve weight loss prior to bariatric surgery.
“One of the things we often say is bariatric surgery is a tool; it’s not the end-all-be-all for weight loss. So it’s really about making sure this tool is used wisely and proactively by our patients and having it work most effectively in the long run,” Hutcheon says.
For future investigations, the researchers hope to explore the impact that presurgery weight-loss programs have on longer term (more than one year) surgical outcomes.




