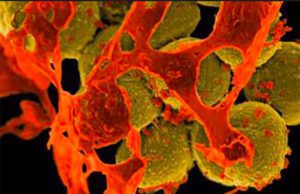
Methicillin-resistant Staphylococcus aureus (MRSA) (Image from FDA)
Philips Healthcare (NYSE:PHG) has combined some of the latest information technologies to help hospitals battle healthcare-acquired infections (HAIs), which can extend a hospital stay, lead to rehospitalization, and even to patient death.
HAIs can have devastating effects on patients’ physical, mental/emotional, and financial health, and they cost billions of dollars in added expenses to the healthcare system. There were an estimated 687,000 HAIs in U.S. acute-care hospitals in 2015. About 72,000 hospital patients with HAIs died during their hospitalizations, according to the U.S. Centers for Disease Control and Prevention.
Recent studies indicate that the incidence of certain types of HAIs has been dropping due to hospital staff efforts, but they’re still a problem. One in 31 hospital patients has an HAI on any given day, according to a CDC estimate. The most common include central line-associated bloodstream infections, catheter-associated urinary tract infections, surgical site infections, methicillin-resistant Staphylococcus aureus (MRSA) and Clostridioides difficile (C. difficile).
Three years ago, Philips set out to fix one of HAIs’ thorniest problems — pinpointing the source of an HAI before it can spread. The company combines data from electronic health records (EHRs) with machine learning and genomic sequencing in its recently launched IntelliSpace Epidemiology platform.
IntelliSpace Epidemiology was designed to automatically collect data from hospital systems, such as patient admissions/discharge/transfer data and laboratory information, to track an HAI to the first patient infected. The platform can tell the hospital staff what bed the patient used in the emergency department, which room they stayed in after admission, and which staff member performed dressing changes. It can also trace the phylogenesis or “family tree” of the pathogen to identify how it was transmitted, according to Dr. Joe Frassica, head of Philips Research for the Americas and chief medical officer for Philips in North America.
The platform’s algorithms can find and highlight possible infection clusters to help organize and automate a hospital’s infection control workflow, according to the company. It overlays a patient’s clinic information with that of a pathogen’s genome to help rule out false-positive infection clusters to save time and wasted mitigation efforts. It also has an on-demand, real-time antibiogram — a report that shows how susceptible strains of pathogens are to particular antibiotics.
Advances in genomic sequencing have made such research less expensive and possible to conduct in real time, according to Frassica.
“We can sequence a bacterium’s entire genome for less than a hundred dollars,” he said in an interview with Medical Design & Outsourcing.
Most hospitals have an infection control department that uses manually driven tools that can make identifying the source of a hospital-based disease outbreak take weeks to months, Frassica added.
“It’s a very manual process done with Excel spreadsheets and people looking manually at the discharge dates, et cetera,” he said. “Our system does all that in real time. We know all of the transactions of care based on this clinical data that we have.”
IntelliSpace Epidemiology is a software-as-a-service platform billed as a subscription model and only available in the United States. A research paper on the platform, titled “A core genome approach that enables prospective and dynamic monitoring of infectious outbreaks,” was recently published in Nature Scientific Reports.
Philips could not have developed IntelliSpace Epidemiology without electronic health records (EHRs), machine learning and genomic sequencing, according to Frassica.
“It’s not something we could have done five years ago,” he said. “This is really cutting-edge, to be building phylogenies and combining it with clinical data.
“The impact of this is just one example of what these technologies can do,” he added. “This was an almost unmanageable problem in hospitals before our ability to do this.”




