Researchers are finding new ways to use artificial intelligence and nanotechnology to enhance treatments, from routine dental techniques to attacking cancerous tissue. At the AVS 65th International Symposium and Exhibition, being held Oct. 21-26, 2018, in Long Beach, California, Dean Ho will present the results of two clinical trials that show how AI-enabled personalized medical treatment for a prostate cancer patient and nanotechnology improved recovery for patients after a root canal.
Nanodiamonds are a Tooth’s Best Friend
Nanodiamonds are so tiny that 100 diamond fragments in a row come to only the width of a human hair. These particles have a unique place in biomedical applications, because they are chemically inert, nontoxic and hard, offering new opportunities for the dreaded root canal.
During standard root canal surgery, gutta percha, a filler, is inserted into the void left by the tooth root to promote healing and maintain the structure of the jaw and gum. Ho and his team developed a nanodiamond-fortified gutta percha (NDGP). The diamond filler proved to be a durable treatment that enabled wound repair in the treated area while preventing reinfection.
“Apical wound healing was unimpaired following NDGP administration,” said Ho, a professor of biomedical engineering and pharmacology at the National University of Singapore. “We found that the materials were well tolerated by the patients.”
The preclinical trial enrolled three patients. Next, Ho and his team will explore the use of NDGP fortified with medications to prevent infection.
Fine-Tuning Drug Delivery for Truly Personalized Medicine
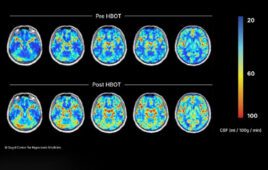
In the second portion of his talk, Ho will discuss the results of a second clinical trial using CURATE.AI, a powerful AI platform that delivers a personalized therapy for advanced, metastatic prostate cancer. The team developed an approach to adjust drug dosing in near real time to optimize every unique moment of the patient’s treatment throughout the therapeutic course.
“Our AI platform, named CURATE.AI, uniquely allows for the immediate identification of drug doses that optimize efficacy and safety,” Ho said.
The research team calibrated the patient’s response to a drug dose using routine testing, like blood draws and imaging, to ensure the best treatment outcome at every point of therapy. The team measured treatment response by measuring the prostate specific antigen (PSA) levels and mapped the progression of lesion metastasis.
“As the patient evolves during therapy, the dosing changes in order to maintain optimal outcomes,” Ho said. “This patient achieved the lowest PSA level reported during the whole duration of the study.”
The results are based on a single patient (N-of-1) clinical trial study. According to Ho, this project is a first for the field of personalized, precision medicine. Following treatment, the patient resumed an active and normal lifestyle.
“The fact that we can achieve a durable response in the patient and completely halt disease progression using AI represents a major advance for the broader field of oncology, as well as drug development,” Ho said.