Biological sex differences can have far-reaching, clinical consequences, as illustrated by organ transplant outcomes. Men and women who receive donated organs can have different rates of transplant rejection, in some cases influenced by the sex of the donor. In general, the influence of biological sex on transplant outcomes has not been rigorously studied and largely underappreciated. A new study by investigators at Brigham and Women’s Hospital assesses what is currently known about the influence of biological sex differences, possible mechanisms that may explain discrepancies between rejection rates for male and female recipients and what questions remain to be explored in future studies. Their analysis is published in Trends in Immunology.
“In solid organ transplantation, the importance and implications of the sex of both the donor and the recipient have long been underappreciated,” says Stefan G. Tullius, MD, PhD, chief of the Division of Transplant Surgery at BWH. “The differences may be subtle but I think they are very relevant, particularly as we move toward individualizing immunosuppression and try to find ways to be more specific in our treatment. I think understanding the relevance of sex differences will play a significant role in this.”
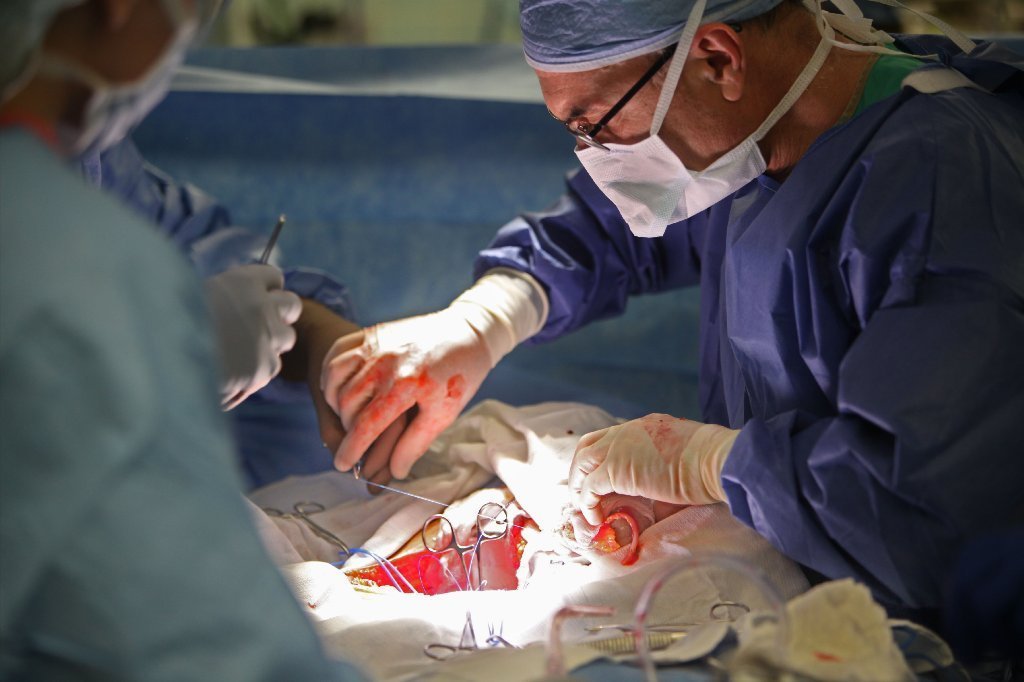
(Image credit: Associated Press)
Transplant rejection is a complicated phenomenon with many contributing factors, and the researchers note that mismatched sex of a donor should not be cause for concern for transplant recipients. However, data on transplant rejection rates have been correlated with specific patterns of donor and recipient sex in several types of transplanted organs, including kidneys and hearts. In kidney transplantation, female donor sex has been associated with an increased rate of transplant organ rejection, especially among male recipients. In cardiac transplantation, female donor organs have also had lower rates of success compared to male donor organs; however, in contrast to kidney transplantation, these differences are only consistently present in male recipients and absent in female recipients. The authors also note the importance of age: Among women 45 and older, they observed a positive effect among female recipients, especially when they received a transplant from a female donor.
Tullius and his colleagues describe two important categories of molecular sex differences that may influence immune response and help account for these different rates: genetics and hormones. Approximately 50 genes on the X chromosome have immunological functions, and may be more variably expressed in females. The Y chromosome, on the other hand, harbors genetic loci for male-specific antigens. Different hormonal environments in males and females may influence multiple immune cell types that express hormone receptors.
The team also notes that certain therapies that target hormone receptors – such as selective estrogen receptor modulators – could be used in the future to target these hormonally-mediated differences between male and female immune responses. Further analysis in experimental and clinical models will be needed to determine if this kind of therapeutic approach may be helpful for organ transplantation.




