The knee is the largest joint in the body and bears five times our body weight with each step you take. Sports injuries, accidents, and arthritis can damage knees and require total knee replacement. This surgery is performed in the U.S. about 580,000 times per year.
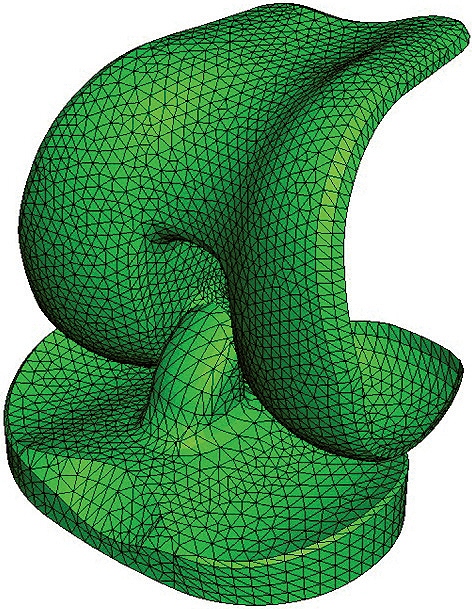
Abaqus FEA models of Smith & Nephew replacement knee components were used for evaluation of the contact between the different parts. The full model (top image) with the original femoral (upper) and tibial (lower) components was used for the sensitivity analysis. The model (bottom image) is modified to study the post-cam contacts.

The American Academy of Orthpaedic Surgeons calls knee replacement one of the most important surgical advancements of the 20th century. The technology continues to evolve since the first artificial knee was implanted in 1968. The current most-used procedure, called total knee arthroplasty (TKA) replaces damaged or diseased joint surfaces of the knee with metal and plastic parts shaped to mimic the function of the original articulation. Sized and shaped to fit, knee implants have been shown to perform well for at least 15 to 20 years in more than 95% of patients, most of whom can achieve a range of motion of from 0 to approximately 120°.
But since the physiological range of motion of a normal knee is a wider 0 to 135°, some TKA patients cannot return to previous levels of full function or activity. Some bones show an atypical response to implantation of the metal. And, as lifespans get longer, the durability of implants becomes increasingly more important. To drive research and innovation and achieve a greater understanding of knee kinematics, improved mobility, and device robustness for knee patients, Smith & Nephew, the U.K.’s largest medical technology company, founded the European Centre for Knee Research in Leuven, Belgium in 2007. Bernardo Innocenti, ME, PhD. is the Centre’s project manager for numerical kinematics.

A test rig in which a knee prosthesis is mounted for the validation of the Abaqus FEA results. The Knee Center testing
team uses Simulia’s Isight optimization software to identify the correct positioning of strain-recording instruments and
the design and ideal thickness of mechanical clamps.
Innocenti and his team use Abaqus Unified finite element analysis (FEA) software from Simulia to estimate rapidly and precisely the effects of different parameters in the design or performance of a TKA. Innocenti said, “When you replace a knee, you are trying to replicate the behavior of biological materials, such as bones, cartilage, and ligaments with non-biological materials such as titanium, stainless steel, and polyethylene. I have everything I need for simulating the performance of all these materials in Abaqus.”
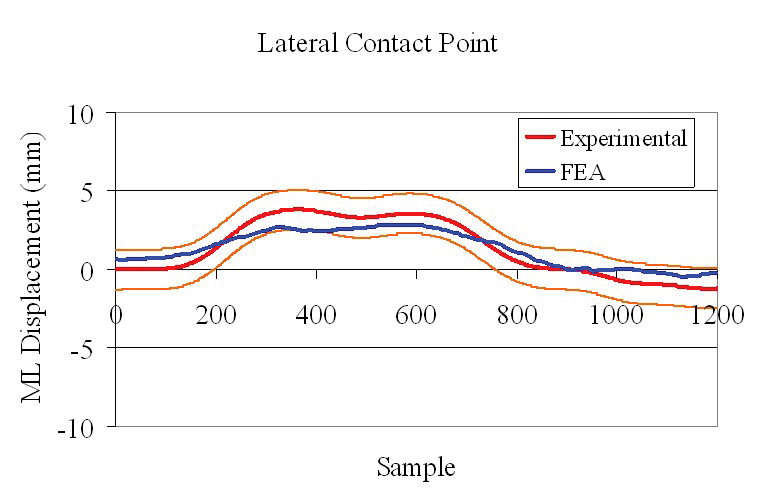
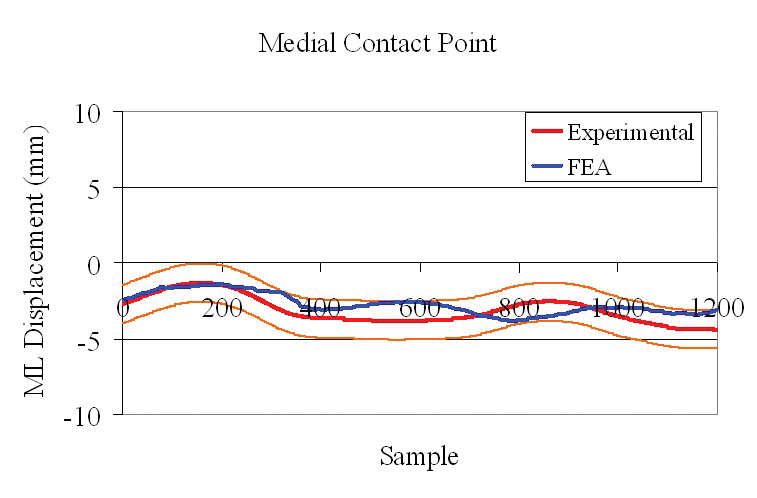
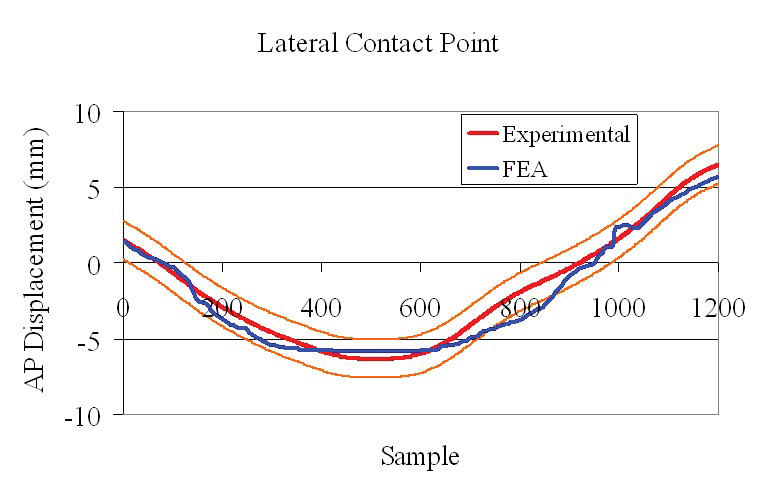
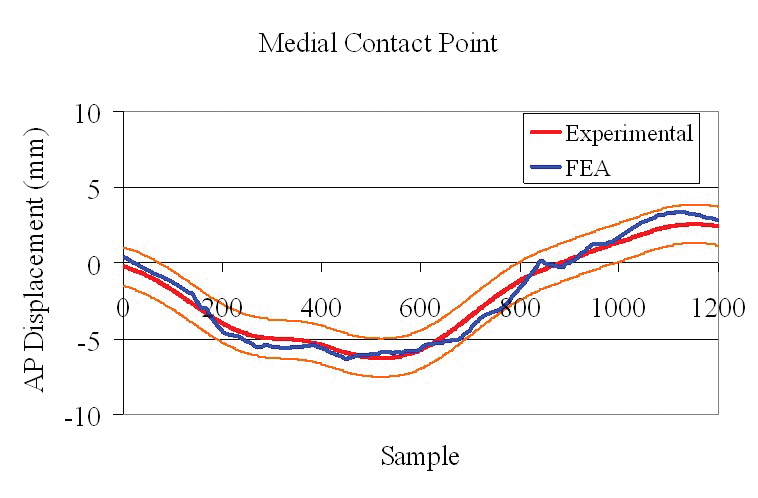
Graphs comparing the pressure centers obtained experimentally (red) and numerically from Abaqus models (blue)
show the accuracy with which FEA predicted results for both lateral and medical contact points between the fibular and tibial components of a knee implant.
A notable problem with modeling the artificial knee is that its mechanics vary greatly over time because as the joint moves, the loads and stresses on the contact points keep changing over the range of motion. Every replacement knee is operating in a unique body environment. Videofluoroscopy of a TKA patient’s leg in motion is an accepted technique for monitoring this functionality. But videofluoroscopy only shows the behavior of the leg bones and metal inserts, not the soft tissues or the polyethylene insert that cushions the contact between the upper and lower parts (the femoral and tibial components) of the prosthesis. This is the challenge that Innocenti and colleague Luc Labey, ME, PhD overcame.
Their study examined five osteoarthritis patients who each received Smith & Nephew’s Journey Bi-Cruciate Stabilized Knee System, a guided motion knee implant specifically designed to produce more natural kinematics after TKA. The patients performed a number of exercises while being analyzed with fluoroscopy – rising-sitting, stair climbing, and step up-down. The resulting kinematics data was used as input for Abaqus FEA models of the knee implants.
Putting the FEA models through the same movement as the patients allowed Innocenti’s team to estimate the contact points between the femoral and tibial components, taking into account the modulating effects of the invisible polyethylene part that is undetectable with videofluoroscopy. The FEA analysis supports the previous contact point displacement measurements derived from fluoroscopy alone but with smoother, more credible and consistent patterns.
For the first time, the models enabled the in-vivo analysis of the contact between the femoral cam and the tibial post. “We validated our technique with experimental results that produced a high quality metric. Our findings can be incorporated into both future design refinements and recommendations we make to surgeons today,” said Labey.
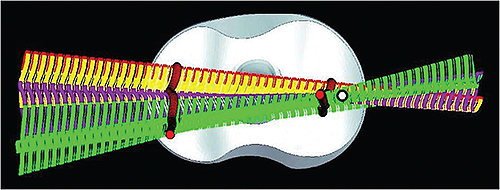
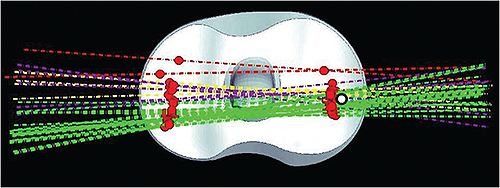
Replacement knee component contact points location (red dots) and contact line rotation (in
different colors according to the corresponding flexion angle) are compared using traditional
fluoroscopy (A) and the Abaqus FEA model with fluoroscopy based kinematics input (B) from a
typical patient during chair rising-sitting. The results support the basic reliability of fluoroscopy, but
also demonstrate the importance of using FEA models for a more realistic estimation of the contact
and for deeper understanding of the loads and stresses that occur
during the in-vivo post-cam engagement.
Validation of their Abaqus models gave Innocenti’s team confidence to extrapolate their data to a wider range of questions about TKA longevity. Innocenti added, “How these materials behave over time is critical to our work because an understanding of wear is very important with prostheses.” Physical prototypes of artificial knees have historically been subject to laboratory wear testing in the same way as many other manmade products. It takes more than one million cycles of knee steps to replicate the wear and tear of a single year of walking. It takes many months to collect enough real-world data to be useful. However, by walking their Abaqus virtual knee prostheses through accelerated test cycles, the Smith & Nephew team can simulate the effects of five years of walking in one week.
Smith & Nephew
www.smith-nephew.com
Dassault Systemes
www.simulia.com
::Design World::




