Getting shots and seeing needles are two events many try to avoid when going to the doctor’s office. Nonetheless, it’s been a way to deliver medication for more than a century. However, pinpointing the exact spot to insert a needle is no easy feat, especially in regions like the suprachoroidal space at the back of the eye. Now, researchers from Brigham and Women’s Hospital have developed a ‘smart’ needle that detects changes in resistance in order to properly and safely deliver medication. The highly sensitive intelligent-injector for tissue-targeting (i2T2) is currently being used in preclinical testing, and the results have been published in Nature Biomedical Engineering.
“Targeting specific tissues using a conventional needle can be difficult and often requires a highly trained individual,” says senior corresponding author Jeff Karp, Ph.D., Professor of Medicine at the Brigham. “In the past century there has been minimal innovation to the needle itself, and we saw this as an opportunity to develop better, more accurate devices. We sought to achieve improved tissue targeting while keeping the design as simple as possible for ease of use.”
As mentioned previously, the suprachoroidal space (SCS), located between the sclera and choroid in the back of the eye, is an extremely difficult location to target with a standard needle. Despite its difficulty, the SCS has emerged as an important location for medication delivery. The challenge arises because the needle must stop transitioning through the sclera, which is less than 1 millimeter thick, in order to prevent damage to the retina. Other common tissue targets include the epidural space around the spinal cord, the peritoneal space in the abdomen, and subcutaneous tissue between the skin and muscles.
The i2T2 device was created using a standard hypodermic needle and parts from other commercially available syringes. While body tissues have different densities, the injector uses the differences in pressure to project needle movement into a specific, target tissue. The driving force, maximal forces, and frictional force of the injector were tested using the universal testing machine. The feedback of the injector is instant, and allows for more precise tissue targeting and minimal overshoot into an undesired location.
“This intelligent injector is a simple solution that could be rapidly advanced to patients to help increase target tissue precision and decrease overshoot injuries. We have completely transformed needles with a small modification that achieves better tissue targeting,” says first author Girish Chitnis, Ph.D., a former postdoctoral fellow in Karp’s laboratory. “This is a platform technology, so the uses could be very widespread.”
In total, the device was tested on tissue from three animal models to determine its accuracy in the suprachoroidal, epidural, and peritoneal spaces. Researchers found that the i2T2 prevented overshoot tissues and delivered medication to the location without additional training.
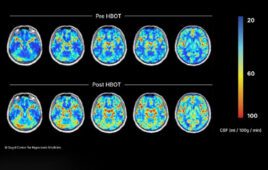
During preclinical models, researchers reported high coverage of contrast agent in the posterior section of the eye, which indicated that the payload had been injected into the correct location. Researchers also showed that the device could deliver stem cells to the back of the eye for potential regenerative therapies.
“The stem cells injected into the SCS survived, indicating that the force of injection and the transit through the SCS were gentle on the cells,” says Kisuk Yang, a co-author and postdoctoral fellow in Karp’s laboratory. “This should open the door to regenerative therapies for patients suffering from conditions of the eye and beyond.”
The researchers plan to continue their exploration of this smart needle’s capabilities and hope to, someday soon, use it on humans.
“The i2T2 will help facilitate injections in difficult-to-target locations in the body,” says Miguel González-Andrades, MD, Ph.D., ophthalmologist co-author of the manuscript and collaborator with Karp’s lab. “The next step toward human use is to demonstrate the utility and safety of the technology in relevant pre-clinical disease models.”