The first randomized controlled trial to directly compare robotic surgery with open surgery for patients with localized prostate cancer finds that robotic and open surgery achieve similar results in terms of key quality of life indicators at three months. The study, published in The Lancet, is the first stage of a two year trial and reports quality of life outcomes such as urinary and sexual function.
Since the use of robot-assisted laparoscopic prostatectomy (RALP) was first reported in 2000, there has been rapid adoption of robotic surgery for men with prostate cancer. One million men are diagnosed with prostate cancer worldwide each year. The most common treatment for localized disease is surgery to remove the prostate gland, and some men experience urinary and erectile problems following surgery. For most men, the operation will get rid of the cancer cells, but for around one in three men, cancer cells may return some time after the operation.
In the USA, 80-85% of prostatectomies are done robotically, and although the proportion is lower in the U.K. and Europe, it is increasing. Robotic surgery is more expensive than open surgery and to date there have been no randomized controlled trials comparing robotic with open surgery.
“Surgery has long been the dominant approach for the treatment of localized prostate cancer, with many clinicians now recommending the robotic method to patients. Many clinicians claim the benefits of robotic technology lead to improved quality of life and oncological outcomes. Our randomized trial, the first of its kind, found no statistical difference in quality of life outcomes between the two groups at 12 weeks follow-up. Patients are now being followed-up for a total of two years in order to fully assess the longer-term outcomes, including on cancer survival” says lead author Professor Robert ‘Frank’ Gardiner, University of Queensland Centre for Clinical Research, Brisbane, Australia. “In the meantime, patients should choose an experienced surgeon they trust and with whom they have a rapport, rather than basing their decision on a specific surgical approach.”
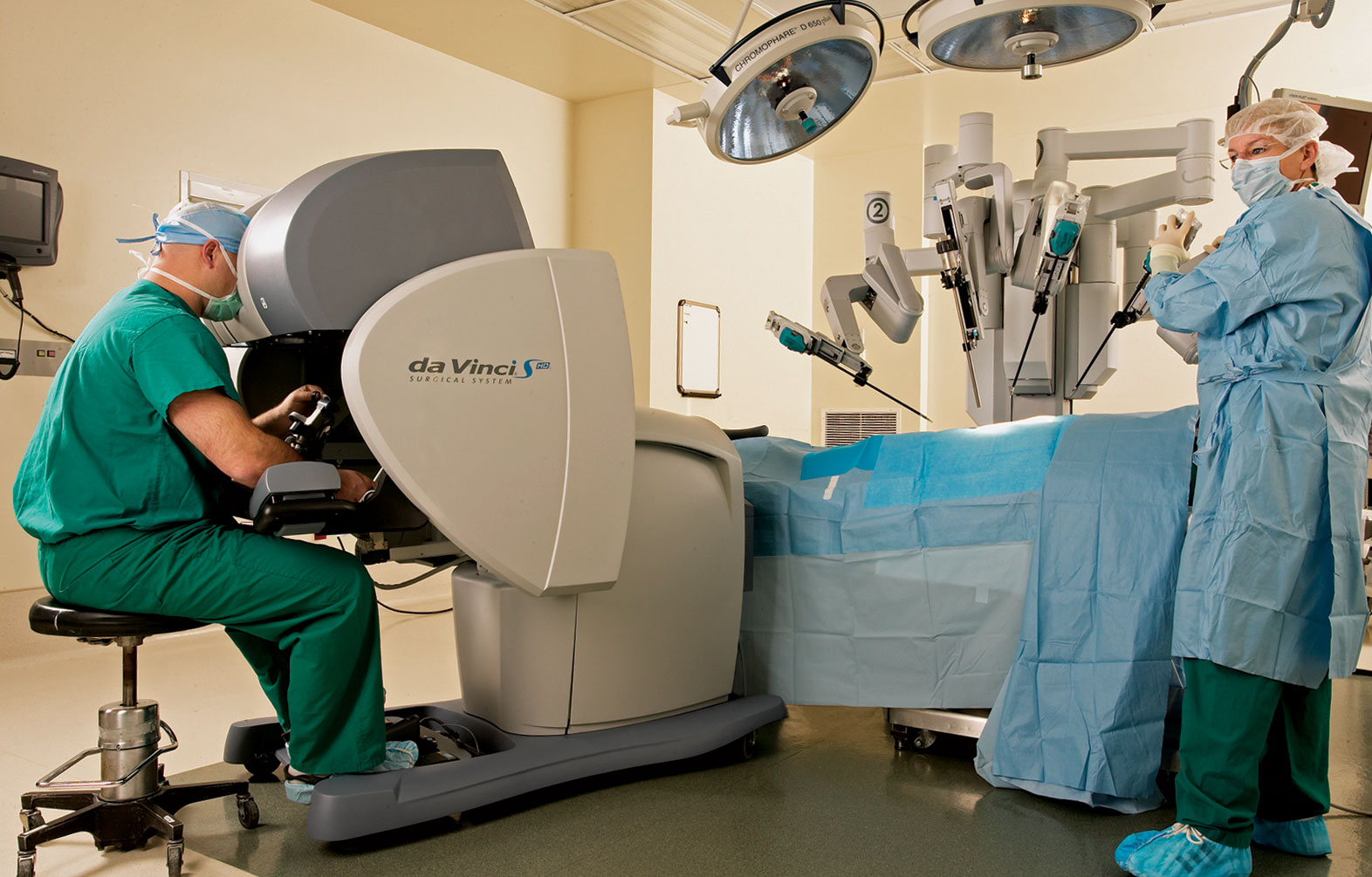
(Image credit: Visage Technologies)
RALP uses a high magnification (x10) 3D camera that allows the surgeon to see inside the patient’s abdomen through a keyhole incision. The camera is attached to one of four arms on the robot – the other three hold other surgical instruments needed during the operation. The surgeon is in the operating room but is away from the patient and controls the robotic arms to perform the operation. Robot-assisted surgery is most commonly used for prostatectomies, but is increasingly being used in gynaecology, cardiothoracics, head and neck, and general surgery, as well as other operations in urology.
The study included 308 men with prostate cancer. They were randomly assigned to either receive robot-assisted surgery (157) or open surgery (radical retropubic prostatectomy) (151). They were then followed up for 12 weeks after the operation. All the operations were led by two surgeons at the Royal Brisbane and Women’s Hospital.
The primary outcomes included urinary and sexual function at 12 weeks and there was no difference between the two groups. There were also no differences in the number of post-operative complications. Patients who underwent open surgery spent a longer amount of time in the hospital after surgery but on average both groups spent the same number of days away from work.
Patients who underwent open surgery lost on average three times more blood (although no transfusions were needed during the operations because blood was recycled back into the patients during the open operations). In the immediate aftermath of the surgery, patients who underwent robotic surgery experienced less pain doing day to day activities (at one week), and reported better overall physical quality of life (at six weeks). Over time, the differences levelled out, becoming non-significant at 12 weeks.
The authors note that urinary and sexual function can continue to improve for up to three years after surgery, so differences in outcomes between these two groups might become apparent later on. The study is the first stage of a two year trial.
Writing in a linked Comment, Professor Ara Darzi, Imperial College London, says, “The clinical community waits with anticipation for the one-year oncological outcomes; the last patient underwent surgery in March, 2015. It will be the interpretation of the longer-term functional and oncological outcomes that reveals the full implications of this study for clinical practice.
Darzi adds, “Trials that show equivalence for an innovation are sometimes interpreted as supporting a return to existing practice, including rediverting the training of a generation of surgeons who might have followed the innovation’s evolution. Equivalence and noninferiority should also be seen as positive, showing the innovation has preserved the intended and well established purpose of surgical intervention, such as good oncological outcomes balanced against acceptable functional side effects. It is these advances in applied technology, reducing the trauma of access and the invasiveness of surgery, that also provide the platform on which to develop adjunct technological innovations towards further improving the quality and safety of surgery. Our challenge as a community is to demonstrate safe and cost-effective translation alongside significant health and economic impact.”




