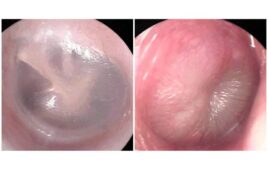
In this image, lung cancer driven by the KRAS oncogene shows up in purple. MIT biologists have found a potential new way to treat this type of lung tumor, long thought to be “undruggable.” [Image from National Cancer Institute / Huntsman Cancer Institute at the Univ. of Utah]
Gene mutations in the KEAP1 gene could help treat mutations in the KRAS gene that causes certain lung cancer types to be undruggable.
KEAP1 mutations occur with KRAS mutations in approximately 17% of lung cancer cases, according to the researchers. The researchers found that cancer cells that had KEAP1 genes want glutamine, which is used for protein synthesis and energy use. If the cells are deprived of glutamine, a treatment for KRAS and KEAP1 mutations may arise.
The researchers found that small-molecule-based inhibitors of glutaminase could slow cancer cell growth and resulted in smaller tumors in lung adenocarcinoma cell lines and tumors in mice who had KEAP1 mutations.
A study revealed a way to figure out which lung cancer patients would respond better to drugs that block glutaminase.
“All cell lines that we have currently tested that are KEAP1-mutant – independent of their KRAS status – appear to be exquisitely sensitive to glutaminase inhibitors,” Rodrigo Romero, first author on the paper, said in a press release.
Lung cancer is the leading cause of cancer death among men and women in the U.S. with about 155,870 deaths expected to happen in 2017. There is expected to be approximately 222,500 new lung cancer cases this year, according to the American Cancer Society.
Lung adenocarcinoma makes up about 40% of lung cancer cases. About 15% to 30% of those cases have a KRAS mutation. KRAS has been known to be hard to prevent, according to the researchers, because ways of blocking the KRAS protein interactions have been unsuccessful.
KRAS mutations usually have another mutation, which often includes KEAP1, the third most frequently mutated gene in lung adenocarcinoma. The researchers wanted to determine how the mutations affected lung cancer progression, so they created KEAP1 mutations in mice using a CRISPR/Cas9 gene editing system to target the gene.
CRISPR/Cas9 screenings showed that lung cancer cells that had KRAS and KEAP1 loss-of-function mutations needed increased amounts of glutamine more than other cells. Researchers tested two glutaminase inhibitors against the cancer cells to see if starving the mutations of glutamine could be a therapeutic vulnerability.
The researchers tested it against a cancer cell compound known as CB-839 that has been in phase I clinical trials for KRAS-mutant lung cancer. The test showed that CB-839 slowed the growth and the tumors were kept at a smaller size than normal in lung adenocarcinoma with KEAP1 mutation.
“There are also many clinical trials testing the efficacy of glutaminase inhibition in a variety of cancer types, independent of KRAS status. However, the results from these studies are still unclear,” Romero said.
KEAP1 protein usually stamps out NRF2, which controls the activation of an antioxidant response that helps remove toxins, reactive oxygen species from cells. The researchers disabled KEAP1 with loss-of-function mutations and saw that NRF2 proteins could come together and form a hyperactivation of the antioxidant response.
According to Romero, lung adenocarcinomas with the EAP1 mutation could use the hyperactivation to promote cellular growth or detoxify intracellular damaging agents.
Genes targeted by NRF2 had a greater expression in advanced stage IV tumors and patients who had up-regulated NRF2 tumors had worse survival rates.
The researchers plan to continue to study several mutations beyond KEAP1 that may work with KRAS in mice models.
“The complexity of human cancer can be quite daunting,” Tyler Jacks, director of MIT’s Koch Institute for Integrative Cancer Research and co-senior author of the study, said. ““The genetic tools that we have assembled allow us to create models of many individual subtypes of the disease and in this way begin to define the exploitable vulnerabilities of each. The observed sensitivity of KEAP1 mutant tumors to glutaminase inhibitors is an important example of this approach. There will be more.”
The research was published in the journal Nature Medicine and was funded by the Laura and Isaac Perlmutter Cancer Support Grant, the National Institutes of Health and the Koch Institute Support Grant from the National Cancer Institute.
(See the best minds in medtech live at DeviceTalks West, Dec. 11–12 in Orange County, Calif.)