The emergence of telerobotics and 5G may expand the reach of highly specialized physicians to parts of the world where no treatment options exist.
Doug Teany, Corindus
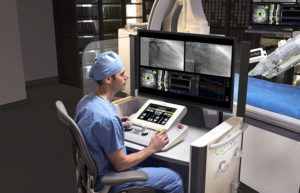
This surgeon works at a CorPath console. (Image courtesy of Corindus)
A 1962 episode of the iconic cartoon series The Jetsons featured Jane Jetson calling the family doctor via a video screen to check on her son Elroy, who showed symptoms of “Venus Virus.”
Nearly 60 years after that episode aired, telehealth has established itself as a disruptive tool for remotely diagnosing conditions. But the advent of the COVID-19 pandemic has thrust telehealth to the forefront, and combining it with other groundbreaking technology will expand its capability beyond diagnostics.
Remote-operated robotics, or telerobotics, represents one of those technologies that can evolve telehealth from a primarily diagnostic tool to something that can treat patients remotely, ushering in a new era of care that we call tele-treatment. By combining existing robotic technology with high-speed broadband internet, telerobotic treatment has the potential to dramatically lower the rate of mortality and morbidity suffered by patients who lack access to timely care. While this may sound futuristic, remote robotic procedures have already made significant progress.
In 2019, Dr. Tejas Patel, chair and chief interventional cardiologist of the Apex Heart Institute in India, conducted the first-in-human telerobotic intervention study. Patel successfully completed five robotic-assisted percutaneous coronary intervention (PCI) procedures on patients who were 20 miles away from him in India, using a hardwired internet connection to manipulate the robot with a set of joysticks and a video monitor. The success of this study paves the way for large-scale, long-distance telerobotic treatment across the globe, which may expand patients’ access to care while reducing their time to treatment.
What 5G means for healthcare
5G is much more than a network upgrade for your cell phone. It’s a massive technological leap that will usher in a transformative era of innovation and creation. Much of the hype around 5G has to do with speed, and while speed is certainly a factor — 600 times faster than the typical 4G speeds on today’s mobile phones — there are significant benefits that extend beyond that. 5G offers greater bandwidth, which means it can handle many more connected devices than previous networks. This will be crucial as the number of internet-connected devices grows in the coming years.
In healthcare, 5G’s speed and low latency means it can support telerobotic interventional procedures in extremely remote parts of the world where hard-wired internet options don’t exist. With acute ischemic stroke, for instance, less than 10% of all patients in the world have access to what is considered the “gold standard” of care, a minimally invasive procedure to remove a clot called mechanical thrombectomy. By expanding the reach of world-class physicians through remote intervention, including 5G-powered intervention, we hope to significantly improve the survival rate for conditions such as stroke and heart attack.
In October 2019, interventional cardiologist Dr. Ryan Madder performed the first multi-city, transcontinental telerobotic test procedures over three network connections, including a 5G network, demonstrating that the technology of the future is in fact here today. Based outside of Boston, Madder successfully completed the test procedures with state-of-the-art vascular simulators in New York and San Francisco. The test demonstrated the viability of telerobotic intervention over a variety of networks and distances up to 3,000 miles that could drastically improve access to care.
The need for tele-treatment
Cardiovascular disease, including heart attack and stroke, is the most common cause of death in the world. Telerobotics represents a major disruptive force in creating treatment options for patients who lack access to care, which is particularly crucial for emergent conditions. For example, in stroke, they say time is brain. Every 90 minutes of delay in care reduces a stroke patient’s disability-free lifetime by one year. And only 55% of Americans live within 60 miles of a primary stroke center. As a result, patients are dying or living with the burden of serious long-term health effects because they did not have access to appropriate care fast enough. The advent of telerobotic intervention will expand the reach of highly specialized physicians to parts of the world where no treatment options exist, significantly reducing mortality and long-term disability rates around the world.
When telerobotic procedures become more widely adopted, the first iteration of this type of tele-treatment will likely take place within the traditional “hub-and-spoke” model of care, in which a physician at a “hub” hospital is directly connected to a robotic system at a second hospital through a secure fiber optics network.
What comes next
The emergence of telerobotics and 5G offer an opportunity to broaden access to care and evolve the traditional hub-and-spoke model by delivering care to patients, regardless of whether they can access a hospital or not. For heart attack and stroke victims who can’t access a hospital, remote intervention may become a life-saving tool in the very near future.
Doug Teany is the chief operating officer of Corindus, a Siemens Healthineers company that works in robotic-assisted vascular interventions. The company’s CorPath platform is the first FDA-cleared medical device to bring robotics to percutaneous coronary and vascular procedures.
The opinions expressed in this blog post are the author’s only and do not necessarily reflect those of Medical Design and Outsourcing or its employees.




