The nation’s transplant network is taking a long-awaited step to ease a serious disparity: Where a patient lives affects whether they get a timely liver transplant or die waiting.
Desperate patients sometimes travel across the country to get on a shorter waiting list — if they can afford it. On Monday, the United Network for Organ Sharing is proposing a change, redrawing the map that governs how donated livers are distributed so patients wouldn’t need to leave home for better odds.
“We want to make sure we give everyone a fair opportunity to get a liver transplant,” says Dr. Ryutaro Hirose, chairman of the liver transplant committee at UNOS, which runs the nation’s transplant system. “It’s pretty much long overdue.”
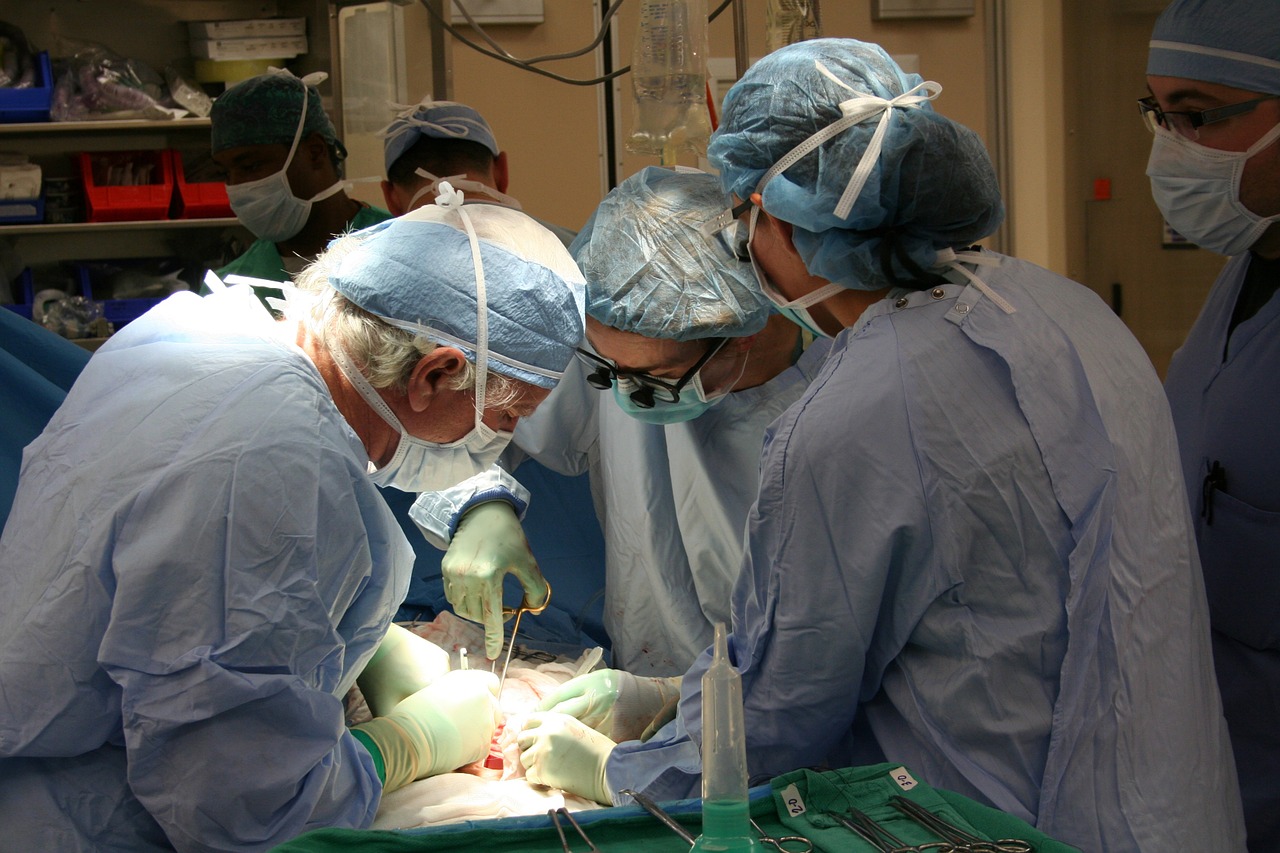
The problem is that some parts of the country have fewer available organs, and higher demand for them, than others. That means someone in California or New York, among the toughest places to get a new liver, tends to be sicker before getting a transplant than someone in South Carolina or Washington state.
“There’s a huge difference in the risk of death on that waiting list depending on where you live,” says Hirose, a transplant surgeon at the University of California, San Francisco. Shifting the boundaries that determine where a liver is offered first “matches better the organ supply and demand.”
More than 14,600 people are on the waiting list for a new liver. Just over 7,100 received one last year — all but a few hundred from deceased donors — and more than 1,400 people died waiting.
The geographic disparity adds another hurdle.
Livers are offered first to the sickest patients as determined by a ranking, a so-called MELD score, which uses laboratory tests to predict their current risk of death. The nation’s 11 transplant regions are subdivided into local areas with individual waiting lists, and there are wide variations in organ availability both within and between regions.
Today, some regions are able to transplant patients before they’re super-sick — with MELD scores as low as 23 — while others can’t provide transplants until a patient’s MELD score reaches 35, meaning they’re at risk of death within weeks, Hirose said.
It’s legal to move around for a better chance, if people know that and are able to. For example, the late Apple CEO Steve Jobs lived in California but in 2009 had a transplant in Tennessee, which at the time had one of the shortest waits.
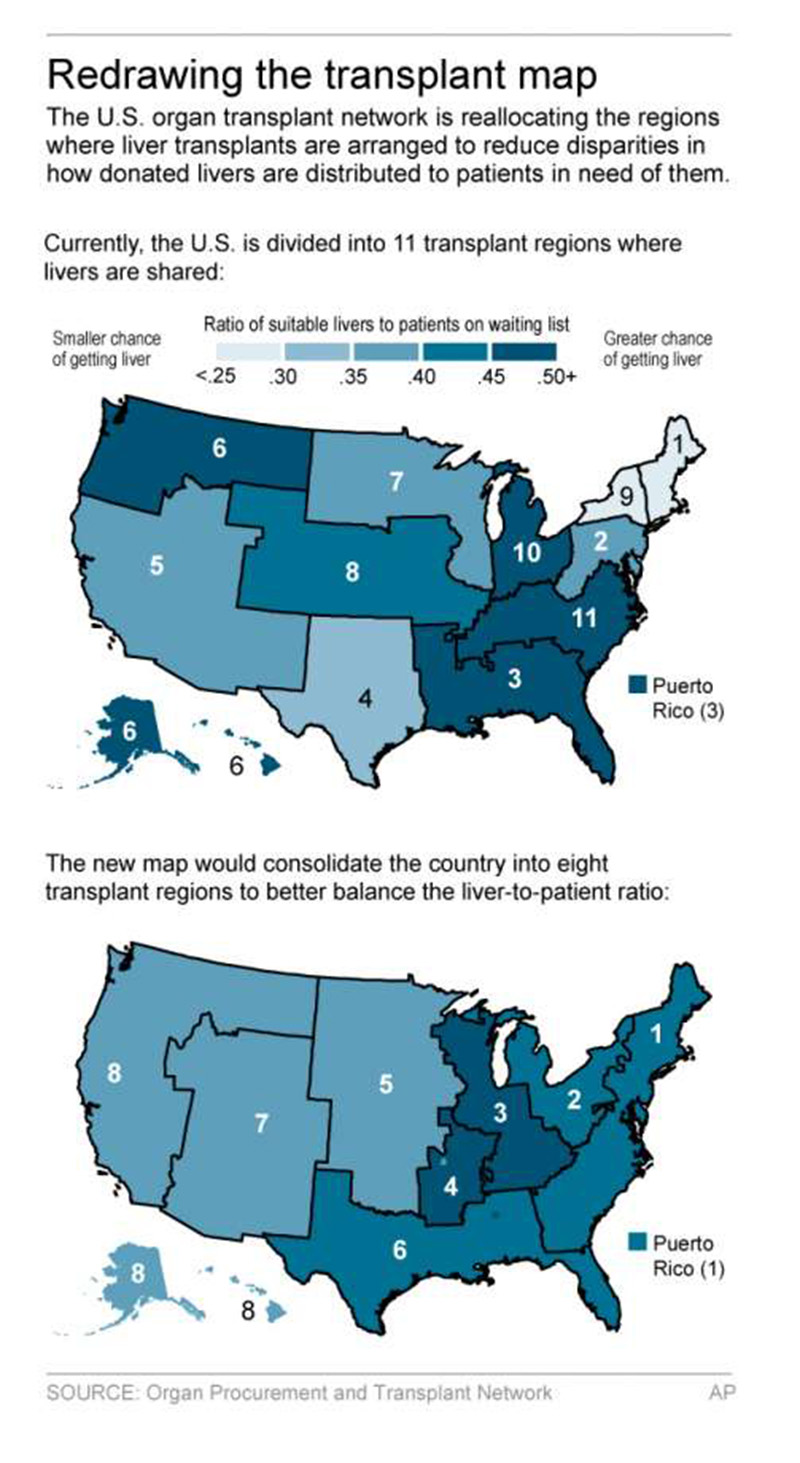
UNOS’ proposed fix is similar to how politicians redraw voting maps: divide the nation into eight new “districts” for liver transplants. That allows wider sharing and shifts the boundaries to better mix areas where more potential donors live with areas that have longer waiting lists.
The goal is for patients to have similar MELD scores at the time of transplant no matter where they live. Research models suggested the change would mean the less sick in some places, such as in the South and Northwest, would wait a little longer so that sicker people elsewhere can get a new organ a little sooner.
UNOS has debated how to change liver distribution for several years, a process Hirose called contentious as some transplant centers with shorter waits didn’t want to lose them. The proposal will be open for comment from the public through mid-October before any changes are finalized.
Sick patients shouldn’t have to leave home to improve their odds of a transplant, says liver recipient Myles Kane. He was shocked when his own doctors in New York urged the Brooklyn man to explore that option after an autoimmune disease caused his liver to fail at age 33.
“There’s this magical window where you have to be the sickest person on the list, but if you die from that sickness — it’s a real narrow window,” says Kane, who eventually got on a shorter waiting list in North Carolina, where his girlfriend’s parents lived.
They gave Kane a place to stay for three months while recuperating from his December 2013 transplant; he met other patients who had to spend months in hotels.
The transplant chief at a leading liver center welcomed the proposed change.
“The distribution of organs is not a right, it’s a gift. We want to try to allocate that gift in the most fair way possible, the way that does the greatest good,” says Dr. Abhinav Humar of the University of Pittsburgh Medical Center, who isn’t part of the UNOS committee.
Because a piece of a liver can regrow, patients can avoid the transplant wait if they’re able to find a living donor, he noted. But ultimately, more organs from deceased donors are needed.
With the proposed remapping, “we’re just changing the way the pie is distributed,” Humar says. “The best solution would still be to make the pie bigger.”




