As hospitals try to maintain effective and efficient operations, physician call systems can be a critical element in maintaining quality medical care and financial stability. In a new report published in The American Journal of Medicine, a decade-long study from a large teaching hospital in Toronto, Canada, shows that a change in staff scheduling resulted in 26 percent higher readmissions, an unintended and negative result.
“Medical practice is a paradox of sustainability and continuity. Sustainability means that one physician cannot be available at all times because of their own personal needs and finite stamina. Continuity means that one patient prefers to have the same physician every time for building understanding and avoiding handover errors. This paradox is pervasive in acute care medicine and particularly important following recent changes to house-staff physician schedules in the United States and Canada. The situation has no simple solution and a better understanding of trade-offs is necessary for thoughtful decision-making,” according to lead investigator Donald A. Redelmeier, MD, of the Department of Medicine, University of Toronto.
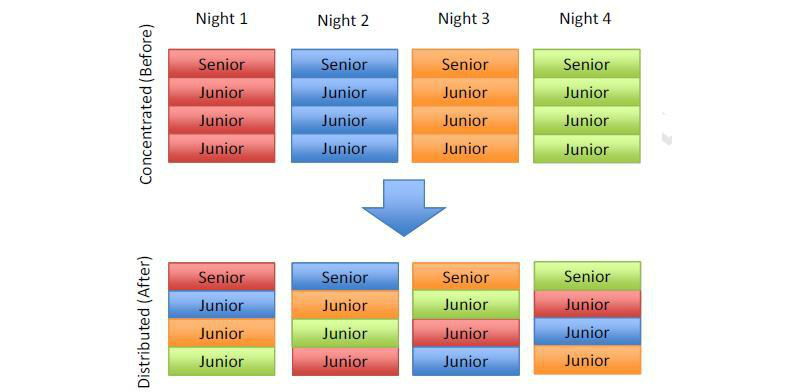
This is a visual representation of physician call systems at Sunnybrook Hospital before and after physician call system change. Each small rectangle represents a resident labeled with their training level. Each color represents a team of residents that cares for the same patients each day. Each collection of 4 rectangles represents a single group of residents on call at night. (Credit: The American Journal of Medicine)
The Sunnybrook Health Sciences Centre is a large teaching hospital with about 10,000 medical inpatient discharges annually. Admissions and patient care are conducted by teams comprised of attending physicians, senior residents, junior residents, and medical students; each team is responsible for 15-25 inpatients. In 2009, the hospital’s Division of General Internal Medicine changed how it organized physician teams. Previously, teams had been deployed using a concentrated or bolus system, which meant that teams remained together throughout a single shift, with four teams covering 24-hour periods. The new arrangement distributed the senior and junior residents across the four shifts.
This distributed system meant that patients could have a team member present every day, theoretically improving continuity of care and decreasing patient readmissions.
The study covered the period from January 2004 through December 2013 and determined readmission rates for 89,697 consecutive discharges, with 37,982 before the call system change and 51,715 afterwards. After correcting for each patient’s likelihood of readmission using an established method (the LACE score), the call system change increased the readmission rate by 30%, and this increase persisted across diverse patients (age, readmission risks, medical diagnoses). The net effect was equal to 7240 additional patient days in the hospital following call system change. There was no significant change in mortality.
As a check on the results, the researchers also examined the readmission risk at a nearby control hospital and found no similar increase during the period.
“Together, the findings show that well-intentioned and well-received changes aimed at improving physician call systems can have unintended, undesirable, and unrecognized consequences,” noted Dr. Redelmeier, who analyzed the data at the Institute for Clinical Evaluative Sciences where he is a core scientist.
Investigators caution that the observed increase in readmission rates does not prove that the distributed physician call system is a failure and needs to be reversed to the concentrated model. The increase in readmission rates was not associated with worsened patient mortality, increased workload imposed on surrounding hospitals, or decreased healthcare worker satisfaction. Dr. Redelmeier emphasized that “Our data suggest that the distributed call system creates a different balance of sustainability with continuity and merits more reconsideration for improvement.”




