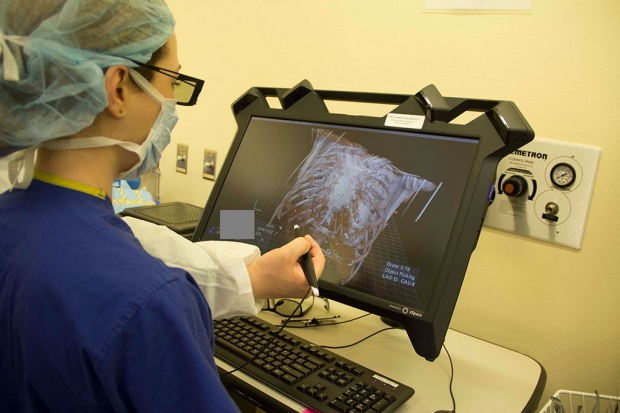
A computer system at Lucile Packard Children’s Hospital Stanford allows medical images to be viewed and manipulated in three dimensions. (Credit: Lucile Packard, Children’s Hospital, Stanford)
When Gina Milner needed a new heart valve, she was surprised to learn that a virtual-reality tool could help her get one.
Milner’s doctors at the Adult Congenital Heart Program, a joint program of Lucile Packard Children’s Hospital Stanford and Stanford Health Care, hoped to perform her valve replacement through a much smaller incision than usual. To figure out if this approach would be safe, surgeon Katsuhide Maeda, MD, used a new computer program that transformed Milner’s CT scans into a 3D image of her heart, lungs and chest cavity. He then donned a pair of 3D glasses and stood in front of a special computer monitor that let him rotate and examine every layer of her cardiothoracic anatomy from any angle. The technology, called True 3D, helped Maeda anticipate what anatomic structures he would see behind a small surgical opening at each stage of Milner’s surgery.
“For patients with very complex anatomy and a lot of variation from the normal cardiac structure, 3D technologies are really helpful,” says Maeda, a clinical associate professor of cardiothoracic surgery at the School of Medicine.
Milner, 46, was born with a heart defect called tetralogy of Fallot that was repaired in childhood, placing her in the group of patients for whom standard 2-D imaging may not give surgeons the information they want. “It can sometimes be very hard to understand how to put a path through the heart,” Maeda says.
Milner’s successful Dec. 2 surgery, the first at Packard Children’s to use the new imaging technology, is one of many examples of how virtual-reality techniques are now helping patients. Her surgery is also one of many recent successes for the Adult Congenital Heart Program, which recently became one of the first in the country to receive formal accreditation from the Adult Congenital Heart Association as a comprehensive care center.
Big view through a small window
Last fall, Milner had difficulty breathing. Testing revealed that she had a leaky pulmonary valve. Blood was backwashing into the pumping chamber on the right side of her heart, making it work too hard. Milner’s heart became dangerously enlarged, and her heart and lungs couldn’t deliver enough oxygen to the rest of her body.
Most patients in this situation need an open-heart procedure to get a new heart valve, and Maeda wasn’t sure if the minimally invasive surgery he wanted to perform instead was feasible. The 3-D technology helped him figure it out before he made a single incision.
“By looking at her CT scans in three dimensions, we were able to tell that we would have enough space to work with,” Maeda says. The technology can also create 3D images from MRI scans.
Some adult congenital heart disease patients have a lot of scar tissue inside their chests from prior surgeries; with the 3D image, Maeda could see that Milner did not. “We could prepare in our minds, if we cut the bone this much, we can get access to this or that blood vessel,” Maeda says. His team also consulted the 3D images during surgery, taking brief breaks in the operating room to double-check the virtual-reality monitor.
Instead of the usual six-inch incision, Maeda was able to perform Milner’s operation through a 2.5-inch incision, enabling her to recover more quickly, causing less post-surgery pain and lowering her risk for complications, such as infection.
Many uses
The 3D innovation will help many of the hospital’s surgical patients, according to pediatric radiologist Frandics Chan, MD, who worked with the Mountain View-based company EchoPixel to develop the new virtual-reality tool using the HP Zvr Virtual Reality Display. (Chan has no financial relationship with either company.)
“In any situation with unexpected anatomy — either anatomical differences the patient was born with, those associated with tumors or those created by a prior surgery — this will be very helpful for both pediatric and adult patients,” says Chan, an associate professor of radiology at the School of Medicine. The team that separated conjoined twins Erika and Eva Sandoval at Packard Children’s in early December used the same virtual-reality technology to help navigate complex steps in the separation, Chan said.
The technique complements 3D printed physical models of patients’ anatomy, which the Stanford 3D and Quantitative Imaging Laboratory produces for surgical planning. The virtual-reality approach has some distinctive advantages. “When you print an anatomical model, you can cut it open once and that’s it,” Chan says. “In virtual reality, you can put it back together, cut it again in a different place and magnify it with the flick of your hand.”
The virtual reality tools will also help train radiologists and surgeons in the diagnosis and treatment of rare diseases, allowing trainees to use an electronic library of 3D disease images to perform virtual dissections.
Breathing easier
At home in Clovis, California, Milner’s recovery is progressing. She’s grateful that the new technology spared her a much larger incision. “For them to have not had to do that is just wonderful,” she says.
She can already feel the benefits of her new heart valve, she adds. “My breathing is so much better.”
“We’re going to use 3D and other virtual-reality technologies more and more,” Maeda says. “They have big advantages for our patients.”




