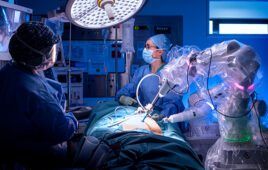
FDA has issued a warning against the use of surgical robots in mastectomies and other surgeries for the treatment or prevention of cancer.
FDA has issued a warning against the use of surgical robots in mastectomies and other surgeries for the treatment or prevention of cancer.
The safety and effectiveness of surgical robots have not been established for use in mastectomies or for surgeries to prevent or treat breast and other cancers, according to the agency, which said it “encourages health care providers who use robotically-assisted surgical devices to have specialized training and practice in their use.”
The warning follows the publication of a study in the New England Journal of Medicine that said robot-assisted cervical cancer surgeries had reduced survival than open abdominal radical hysterectomies among women with early-stage cervical cancer. The journal article noted that other researchers have reported no statistically significant difference in long-term survival when these types of surgical procedures are compared.
Separately, a New Jersey hospital suspended robot-assisted mastectomy after it publicized two such procedures performed by one of its surgeons, concluding that the surgery needs further review, according to a report in the Asbury Park Press. Long Island, N.Y.-based Northwell Health also touted the robot-assisted double mastectomy performed on a woman who carried the BRCA gene, which is associated with developing breast cancer.
Advocates of such robot-assisted surgery say it’s less invasive and causes less pain and fewer scars for patients. Critics such as Hooman Noorchashm, a Philadelphia-area surgeon-turned-patient-advocate, say that robot-assisted procedures are very different from standard surgery.
“If you’re dramatically changing existing standards of care… you better demonstrate that it’s not inferior to existing standards before you advertise it,” Noorchashm said in an interview with Medical Design & Outsourcing.
Demonstrating non-inferiority would traditionally require clinical trials comparing the outcomes of robotic-assisted versus standard surgery. Such studies on breast cancer patients are underway in France and Italy, but none have occurred in the United States. French investigators are comparing outcomes using traditional surgery and Intuitive Surgical’s da Vinci Robot Xi, according to the trial’s listing on clinicaltrials.gov.
“To date, the FDA’s evaluation of robotically assisted surgical devices has generally focused on determining whether the complication rate at 30 days is clinically comparable to other surgical techniques,” the agency’s warning says. “To evaluate robotically-assisted surgical devices for use in the prevention or treatment of cancer, including breast cancer, the FDA anticipates these uses would be supported by specific clinical outcomes, such as local cancer recurrence, disease-free survival, or overall survival at time periods much longer than 30 days.”
The agency has not granted marketing authorization for any robot-assisted surgical device for use in the United States for the prevention or treatment of cancer, including breast cancer. The labeling for robotic surgical devices that are legally marketed in the United States includes statements that cancer treatment outcomes using the device have not been evaluated by FDA.
“Health care providers and patients should consider the benefits, risks and alternatives to robotically assisted surgical procedures and consider this information to make informed treatment decisions,” the agency’s warning said.
The industry leader in robot-assisted surgery, Intuitive promotes the use of its robots for hysterectomies, both benign and cancer-related, on its website. The company does not list mastectomy among da Vinci’s recommended procedures and FDA did not mention Intuitive or any other surgical robotics company in its warning.
“Minimally invasive surgical devices, including robotic-assisted surgical systems and laparoscopic surgical tools, are cleared by the FDA for specific procedures, such as prostatectomy and hysterectomy, not specifically for cancer prevention or treatment,” Intuitive Surgical said in an email. “To date, there are more than 15,000 peer-reviewed articles that, in aggregate, support the safety and effectiveness of robotic-assisted surgery. We value the FDA’s role in protecting and promoting public health, and will continue to look to the agency for guidance as we develop innovative solutions for surgeons and their patients.”
A Danish study published this week in JAMA Surgery said that the risk of severe complications among early-stage endometrial cancer patients who underwent surgery after the national introduction of minimally invasive robotic surgery was significantly reduced. The patients with better outcomes included those whose procedures were minimally invasive laparoscopic surgeries and those who underwent robot-assisted surgeries. Patients were followed for 90 days post-procedure.
Intuitive Surgical recommended that surgeons discuss all treatment options with their patients and that patients ask surgeons about their training, experience, and patient outcomes.
Noorchashm’s wife, Dr. Amy Reed, died in 2017, four years after a myomectomy of fibroid tumors using a power morcellator. The tumors turned out to be a malignant form of cancer called uterine sarcoma that’s difficult to distinguish from benign tumors.
Noorchashm said he’s not anti-innovation but wants surgeons to proceed with caution. “They should slow the hell down,” he said.