(Credit: Monteris Medical)
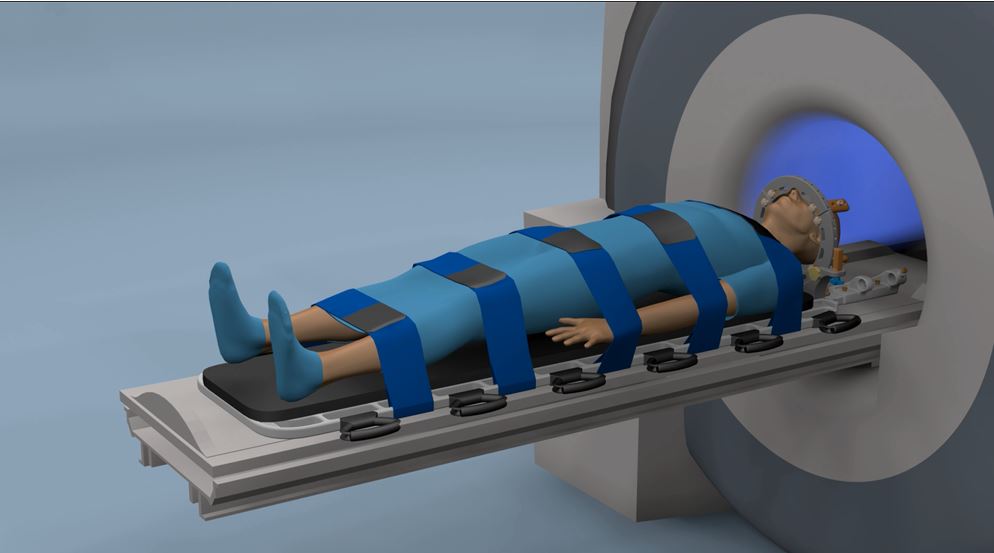
Monteris Medical announced new data were presented supporting the use of its NeuroBlate System for brain lesions at the 2017 American Association of Neurological Surgeons (AANS) Annual Scientific Meeting. The AANS scientific program, taking place from April 22-26, included presentations from three separate Monteris-sponsored studies.
Presenting on Monteris Medical’s LAISE study results, Andrew Sloan, M.D., F.A.C.S., Professor & Vice-Chair, Department of Neurosurgery and Director, Brain Tumor & Neuro-Oncology Center, University Hospitals Cleveland Medical Center, delivered an oral presentation titled “Laser Ablation in Stereotactic Neurosurgery (LAISE): A Multi-Institutional Retrospective Analysis of LITT for Glioma” which described the results of 97 patients whose lesions were ablated with the NeuroBlate System. Of the lesions analyzed, 48 percent were deep-seated, 57.8 percent were considered inoperable, and 1 percent were not suitable for chemotherapy. Also presented by Dr. Sloan and his co-investigators was a poster – recognized among 1,000 submissions with the Third Place Tumor e-Poster Award – titled “Laser Ablation in Stereotactic Neurosurgery (LAISE): A Multi-Institutional Retrospective Analysis of LITT for Brain Metastasis” describing results of 40 patients. These two presentations represent results from patients who had brain lesions ablated from 2011–2015 at nine US centers.
(Credit: Monteris Medical)
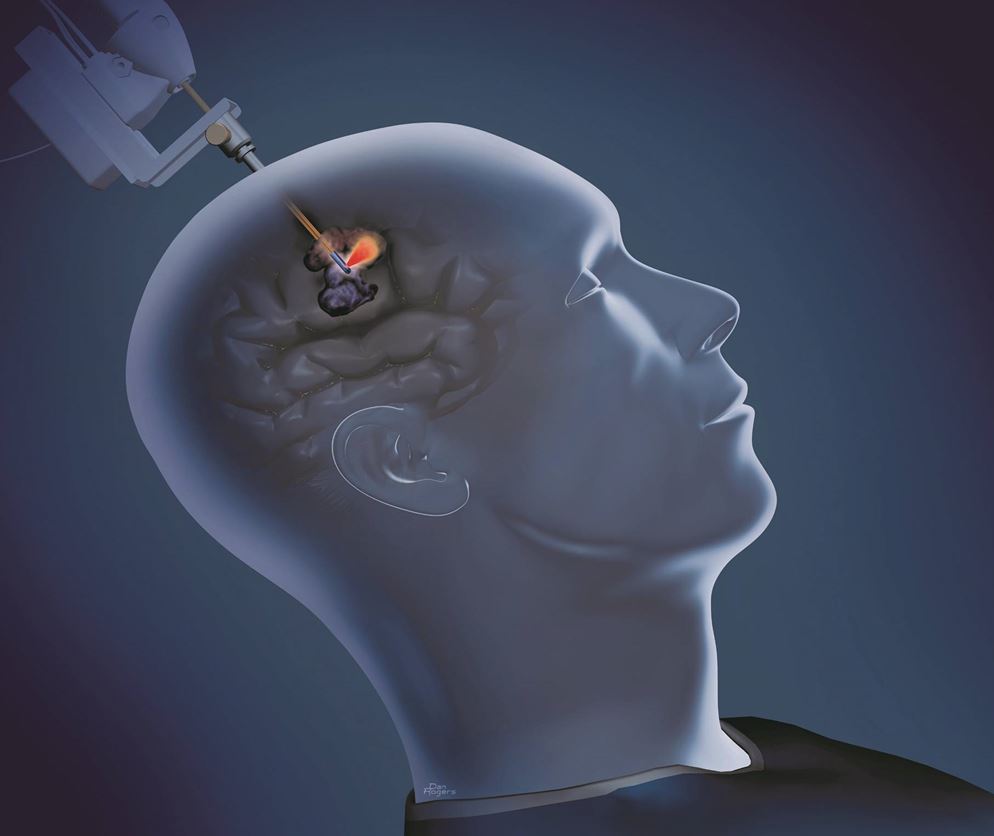
“LITT is a minimally invasive tool used to ablate soft tissue and lesions in the brain that have historically been challenging to access,” says Dr. Sloan. “These encouraging findings from the LAISE study offer preliminary evidence that NeuroBlate may be a viable solution in individuals whose tumors were previously considered inoperable.”
A separate prospective study, titled “Laser Ablation After Stereotactic Radiosurgery (LAASR) – Results of a Multi-Centered Prospective Study Stratified by Pathology,” examined the use of laser ablation on patients’ progressive brain lesions following prior stereotactic radiosurgery. Among 42 individuals receiving laser ablation between October 2012 and December 2015, 19 had biopsy-confirmed radiation necrosis, 20 had recurrent tumors and three had no biopsy.
(Credit: Monteris Medical)
“Approximately 15 percent of patients with brain metastases initially treated with stereotactic radiosurgery will have clinically significant tumor regrowth or radiation necrosis within 18 months, which can ultimately lead to neurological deterioration,” says Veronica L. Chiang, M.D., Associate Professor of Neurosurgery and of Therapeutic Radiology, Yale School of Medicine; Director of Stereotactic Radiosurgery and Medical Director, Gamma Knife Center at Yale New Haven Hospital. “The findings of the LAASR study suggest that LITT has utility on these types of lesions and should be considered for appropriate patients.”

(Credit: Monteris Medical)
Lastly, Dr. Clark Chen, Director of Stereotactic and Radiosurgery and Vice-Chairman of Academic Affairs at the University Of California San Diego Department Of Neurosurgery, presented two posters on data from Monteris Medical’s prospective multi-center registry (LAANTERN). The posters titled “Laser Ablation of Abnormal Neurological Tissue using Robotic NeuroBlate System (LAANTERN): Procedural Safety and Hospitalization” and “Clinical Utilization of Stereotactic Laser Ablation (SLA): an Analysis of the Multi-center Prospective Registry, LAANTERN” provide initial data on the first 50 patients enrolled in this ongoing study.
“The data presented at the AANS Annual Meeting supports NeuroBlate’s potential in addressing brain lesions that historically have not responded well to standard interventions,” says Daryle Petersen, Vice President of Clinical Affairs at Monteris Medical. “We are excited to present our first data extract from LAANTERN, our ongoing multi-center prospective registry on laser ablation. Open, frequent communications are vital to the success of any registry and we look forward to sharing results on this novel, minimally invasive technology at future meetings.”
