The use of advanced molecular diagnostic technologies, such as Next-Generation Sequencing based gene panel testing, to select targeted therapies in advanced cancer patients is known as precision oncology.
In order to evaluate the impact of precision cancer medicine beyond the PFS window and to determine the degree to which any survival or cost advantages persisted, they conducted a follow up analysis on the subset of 44 patients from the original study to measure overall survival, average total healthcare costs, and resource utilization over the entire observation period, from the start of the study through either death or last observed encounter.
Building on a matched cohort study of 44 patients with metastatic cancer who received all of their care within a single institution, researchers from the Precision Genomics & Navican Genomics at Intermountain Healthcare and the Division of Oncology, Department of Medicine, at Stanford University School of Medicine evaluated the overall survival and healthcare costs for each patient.
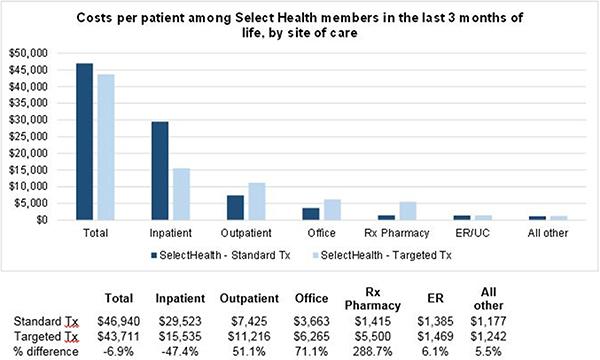
A separate analysis of 1,814 patients with late-stage cancer diagnoses found that those who received a targeted cancer treatment had 6.9% lower costs in the last 3 months of life compared with those who did not.
“In particular, inpatient costs were 47.4% lower for targeted patients during that period, which offset higher outpatient, office, and prescription drug costs.”
Dates of death were available for all 22 patients in the control arm, and for 18 patients in the targeted treatment arm. Patients in the precision medicine group received targeted therapy based on genomic profiling and a molecular tumor board interpretation, while patients in the control group received standard molecular testing indicated for their disease type.
Within the control group, one patients post-PFS survival period had a significant impact on the overall median; this patient survived 187 weeks after the PFS period, more than 400% greater than the next highest value within the control group.
Average costs per week over the entire period were significantly lower for the targeted treatment group compared with the control group.
Moreover, resource use intensity for patients in the targeted group was lower in both higher-cost, acute settings such as inpatient and ER as well in the lower acuity outpatient setting, compared to control patients.
CREDIT: LINCOLN D. NADAULD
