The carbon fiber legs or “blades” used by lower limb amputee runners have arguably become one of the most iconic symbols of the Paralympic Games. Although different lower-limb sports prostheses are used for running, jumping and other activities, they share a single common aim: they are designed to help Paralympians run faster, jump higher or further than other competitors. Form follows function.
For those who have prostheses for more everyday uses, however, their replacement limbs need to be able adapt to different scenarios and perform a variety of functions, not just excel in one discipline—just like an actual leg. So how can we make prostheses feel more like the real thing rather than a specialist tool?

One of the iconic symbols of the Paralympic Games. (Photo credit: Shutterstock via The Coversation)
Whereas modern running blades have a distinctive hook shape, one of the most promising engineering approaches for everyday prostheses is to closely model the biological design of a leg, ankle and foot. This approach is referred to as “biomimicity“.
A “passive” ankle-foot prosthesis generally uses elastic like a spring to replicate the behavior of the Achilles tendon, storing elastic energy and releasing it before ankle push-off. “Active” prostheses additionally use an actuator or motor to make up for the power previously provided by the calf muscle at every step. Such prostheses have been shown to help users walk more like a non-amputee and improve symmetry between the biological and the artificial limb. At the moment, this mainly applies to walking overground at steady speeds rather than activities such as climbing stairs.

For more everyday uses, replacement limbs need to be able adapt to different scenarios. (Photo credit: Shutterstock via The Conversation)
Simple design, advanced technology
Other ways to make a prosthesis more like a biological leg and improve the user’s comfort are more simple. They also illustrate how important it is to involve the amputee in the design process. One user of the most advanced bionic ankle currently available told me its greatest feature was not that it provided a powered push-off or that it allowed them to walk more like a non-amputee. Instead it was that the foot dropped flat on the ground when sitting with an outstretched leg, rather than sticking up awkwardly at a 90-degree angle (as is the case for the majority of prosthetic feet).
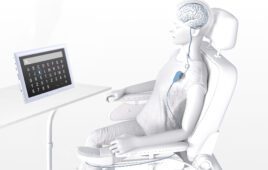
Another issue is how the prosthesis is controlled. Active prostheses now include on-board computers to control the motors and emulate human walking. Prostheses are effectively becoming more and more like wearable robots. What’s more, we can even use interfaces that read signals from the brain or muscles so that the user can operate the prosthesis like a real leg just by thinking and moving in their normal way. The next step being trialled is the use of implantable electrodes that send signals to the brain to give the user tactile feedback so they can feel the contact on the prosthesis as if it were their biological limb, closing the human-machine loop.
These technological and scientific advances connect the amputee more intimately with their prosthetic limb, meaning we can now focus more on how the prosthesis is embodied. In other words, to what extent does the prosthetic limb feel like part of the biological body? Does your brain treat it as such?
We have a good understanding of how our body is mapped in our brain. Both our motor cortex—the movement control centre, if you like—and the somatosensory cortex where we process a wide range of touch sensations are organised somatotopically. This means each area of our body corresponds to a specific area of the primary motor and sensory cortices. Importantly, this mapping does not disappear after the loss of a limb.
This means we have an opportunity to connect prostheses, through muscles and peripheral nerves, to the parts of the brain that would have controlled and sensed the biological body part. But it may also allow us to measure embodiment, how successfully the brain accepts the prosthesis as part of the body.
Ultimately this line of research, bringing together cognitive neuroscience and biomedical engineering, is not only important for designing better prostheses. It is a unique window for understanding how our brain creates and maintains the image of our bodies – mechanisms that apply equally to amputees and non-amputees.
This article was originally published on The Conversation. Read the original article.
(Sources: The Conversation and MedicalXpress)