As we age, proteins in the lenses of our eyes start misbehaving: They unfold and congregate in clusters that block, scatter and distort light as it passes through the lens. A cloudy area, or cataract, forms. In a new study, scientists found that throughout our lifetime, levels of a key protein decline, and may be an early warning sign of a developing cataract. The study, conducted by scientists at the National Eye Institute and the Wilmer Eye Institute of Johns Hopkins Hospital and published online in Ophthalmology, suggests that there is a window before cataracts develop when there may be time to intervene and prevent them.
While cataract surgery is an effective treatment, its cost and the lack of well-trained surgeons limit its availability in many parts of the world, making cataracts the leading cause of blindness.
The protein at the center of the study, alpha-crystallin, is a major structural protein that, under healthy conditions, forms a transparent lattice in the lens. It also acts as a chaperone, binding with other lens proteins that are starting to misfold, which stabilizes them and deters them from clumping together. We’re born with a finite amount of alpha-crystallin, which doesn’t pose a problem in our early years. However, over time, this supply of alpha-crystallin diminishes, and it may not be enough to keep pace with the unfolded proteins that accumulate in the lens as we age, said the study’s lead investigator, Dr. Manuel B. Datiles, III, medical officer and senior clinical investigator at NEI.
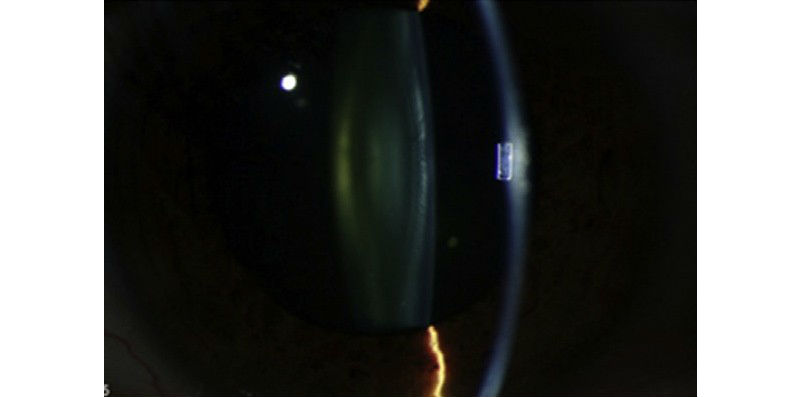
The level of alpha-crystallin declines as cataract progresses. This image shows the left eye of a patient with an early cataract. (Credit: National Eye Institute)
Dr. Datiles and Dr. Walter J. Stark, professor and chief of the cataract and corneal diseases program of the Wilmer Eye Institute, studied this loss of alpha-crystallin over time by measuring levels of the protein every six months among 45 people, age 34 to 79, (66 eyes). All participants had sought eye exams or treatment for suspected cataract.
After a mean of 19 months, the researchers found that cataract progression was far more rapid in lenses with the lowest baseline levels of alpha-crystallin, or the higher rates of alpha-crystallin protein loss, compared to those lenses with the highest baseline levels of alpha-crystallin or slowest rates of loss. By the researchers’ forecast, those with the lowest baseline levels of the protein would be at the highest risk for needing cataract surgery within four years.
The researchers measured and monitored alpha-crystallin levels using a fiber optic-based technology called dynamic light scattering, initially developed to conduct fluid physics experiments in space. Dr. Datiles collaborated with Dr. Rafat Ansari, a physicist, and his team at the National Aeronautics and Space Administration’s (NASA) John H. Glenn Research Center in Cleveland, Ohio, to adapt the device so they could detect alpha-crystallin noninvasively in a living person. Prior to this development, the only way to study these lens proteins was by grinding up the excised lens in the laboratory. Conventional eye exam equipment, such as a slit lamp, is unable to measure proteins in the lens, but merely shows whether the lens is clear or cloudy.
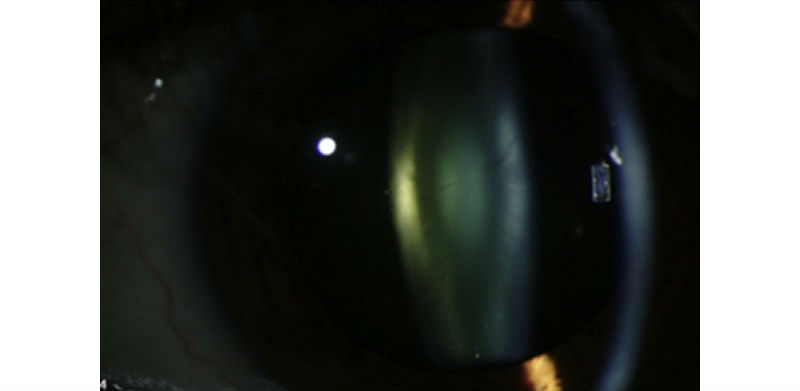
After 20 months, the same eye has a clinically significant cataract. During that period, the level of alpha-crystallin decreased by more than 94 percent. (Credit: National Eye Institute)
The findings help scientists better understand how cataracts form and suggest potential targets for new therapies. Alpha-crystallin appears to be depleted in the process of acting as a chaperone, so supplementing it before levels get too low may be a viable prevention strategy. But since alpha-crystallin protein is itself too large to be delivered via eyedrops, NIH-funded researchers are trying to identify pieces of alpha-crystallin that may act as a kind of mini-chaperone with a similar anti-cataract effect. Dynamic light scattering may also be used to study the effect of some new potential anti-cataract medications recently reported to reverse cataracts in animals and lenses in tissue culture when these medications are ready for human testing in the eye clinic.
Dynamic light scattering might also be helpful in clinical trials of new medications that were shown to cause cataracts during pre-clinical animal safety testing, Datiles said. It may also help with earlier detection of other eye disorders such as presbyopia, the forty-something phenomenon when tasks requiring close-up vision become difficult as the lens becomes stiff and unable to focus light as effectively as it once did. Preliminary evidence from human lens studies in the laboratory suggests that alpha-crystallins are involved in presbyopia.
Although the dynamic light scattering technique is currently used only for research, Datiles said that he can envision it being used in future clinical practice as a way of evaluating people for their risk of developing cataracts and presbyopia. The cost of the device would need to drop significantly. However, much the way creatinine levels are used to monitor kidney function in people at risk for kidney disease complications, if measuring alpha-crystallin became economically feasible, it would provide a biomarker to monitor the health status of the lens, a kind of early warning system that lifestyle changes or other interventions are warranted.




