Operating rooms are one of the highest revenue generating departments in a hospital. They are also one of the most expensive areas of a hospital’s operations. Supplies account for more than 50 percent of a perioperative department’s total expense budget.
Inefficient practices of tracking supplies create the opportunity for significant waste. A Johns Hopkins report found that major hospitals across the United States collectively discard $15 million a year in unused operating room surgical supplies.
As reimbursement for surgical procedures decline, hospitals will be forced to take a closer look at their inventory supply management with the objective of reducing costs through process improvement and the elimination of waste.
Many hospitals face several fundamental challenges when it comes to perioperative supply management. The following are just a few basic issues:
Inventory mix issues: Hospitals do not always have minimum/maximum par levels or re-order points which often results in having too much of some supplies and not enough of others. Additionally, they may have significant duplication of inventory as a result of a poorly designed case pick areas and too much manual inventory controls.
Inefficient case pick area design: Sometimes the wrong storage systems are utilized which can result in open or dead space between shelves and wrong bin sizes and styles. Very often, high density or track systems are deployed in case pick areas based on a preconceived notion that these systems always utilize space more effectively versus traditional shelving racks and bin systems. This can result in a more complicated case pick process with staff spending more time and effort supporting supply management replenishment and case pick activities.
Lack of inventory management technology: Hospitals often lack the necessary technology that provides accurate component demand and appropriate re-order points and requisitions. Inventory management systems may be in place; however, not all of the available features and applications have been installed and utilized. This often leads to manual intervention and excess inventory.
When the right supplies are not on hand, it can impact staff productivity, patient care time, case cart accuracy, and overall cost.
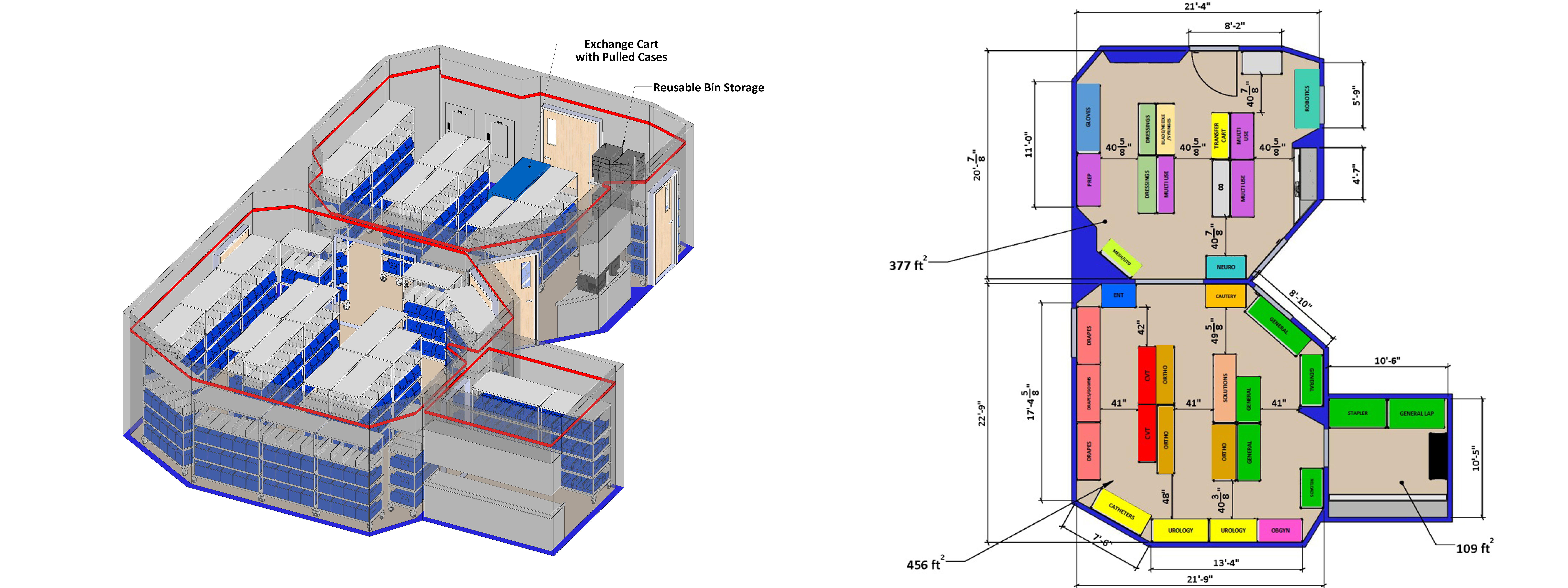
Medline and Wes-Pak created a 3D view of Hardin Memorial Health’s new OR storage system to help staff visualize the storage room once implemented and to validate the selection of proposed storage systems. They also created a new layout which included color coding designed to help staff locate specific types of supplies.
Hardin Memorial Health, located in Kentucky, learned first-hand how inventory management can impact supply management efficiency.
When Linda Bottorff took over as director of supply chain at the hospital, which performs roughly 100 surgeries per day, she quickly realized they needed a better grasp on the number of supplies they had on inventory.
“Quite often we’d run out of supplies,” explains Bottorff. “We would think we had 30 of something on hand when there were none.”
Motivated to implement a change that would drive greater efficiencies, Bottorff turned to Medline and its partner, Wes-Pak Consulting and Design, to take an in-depth look at their perioperative supply management, including the surgical procedures performed, supplies being used, and supplies being pulled and held for possible use.
The case pick room layout was developed in a 3D drawing to reflect current process. From there, Medline and Wes-Pak created a detailed plan, including 3D drawings of their new case pick area to streamline their supply management and improve the overall process, as well as re-established accurate par levels based on documented usage data.
Within one year of implementation, Hardin Memorial Health reduced its on hand inventory investment by more than $500,000 and improved the inventory turn ratio from 2.6 to 7.8.
“New products no longer get into our facility without first going through an in-depth analysis,” Bottorff says. We look at what the product usage will be, the financial increase or savings, what the new product will do that the old one doesn’t. We want to have a deep understanding of how the new product will impact operational and patient care outcomes.”

Hardin Memorial Health’s OR storage room is organized with appropriate signage, and each storage bin is filled to the appropriate par level. All the correct item information is included on each label for item management.
There are several strategies to consider when implementing new perioperative inventory management practices. The following are a just few basic approaches to consider when tackling supply management process improvement:
Establish Champions: Either internally or through a partnership with an outside resource, the best approach to establishing and maintaining control of a perioperative supply management process is to have the necessary expertise to perform the detailed component analytics; understand usage history and develop alternative case pick designs. From there, develop a plan for proper case pick flow and storage devices to sustain the improved process.
Identify Slow Moving or Inactive Components: You should avoid creating par levels for supplies not used. Take the opportunity to clean up the item master and get rid of inactive or slow move products.
Re-engineer the Current Surgical Packs: The cornerstone to most perioperative supply management programs are the surgical packs. All too often these go for extended periods of time before the contents are reviewed and updated to reflect current practice. Bi-annual reviews will help to eliminate waste, maintain a robust surgical pack program and minimize the case pick activities. Comparing the OR surgical procedure case mix with the surgical pack program twice per year will help identify potential gaps in the surgical pack program and will identify potential product waste.
Proper inventory management can be complex, with many variables. Sound practice is also crucial to ensuring the operating room is running smoothly.
Healthcare is not getting any easier, so it is important to take the time to look at these initiatives. Having a plan in place to address supply management challenges will help streamline the OR and ultimately allow staff to worry less about supplies and allow more time with patients.
Ron Evans is the Southeastern Vice President of Perioperative Consulting Services at Medline. In his role, Evans leads a team of consultants equipped to perform LEAN Assessments and work with clients to establish efficient and cost effective supply management systems for Hospitals and Surgery Centers.
A version of this article appeared in the March/April 2018 issue of Surgical Products.




