Patient flow and care management within the perioperative environment is a precise juggling act for every surgical case — people, places, and things. One ball dropped can lead to cascading delays, staff overtime, or even mistakes that impair the outcomes.
Layering an automated workflow process onto surgical patient care reduces variability and standardizes quality by enabling coordinated teams and workflow predictability.
Using technology automates and supports perioperative workflow by streamlining processes, improving consistency, and enhancing patient safety. It also provides opportunities to integrate clinical patient and event-driven data into visual displays to improve team communication, focus on the patient, and analysis of OR utilization.
For example, visual dashboards in perioperative areas enable real-time patient tracking and status updates. Integration with secure networks automates communication across care teams both inside and outside facilities.
Leveraging real-time data captured from automated workflows allows hospitals and surgery centers to use analytics to measure, sustain, and improve surgical efficiency and clinical quality as well as quantify success against key performance indicators such as block utilization, cancellation rates, first and subsequent on-time starts, turnover times, and patient safety metrics.
Planning for Surgery
LiveData PeriOp Manager integrates real-time data with workflow automation to coordinate and manage patient care through the surgical journey.
The journey starts before the patient enters the operating room at a hospital or ambulatory surgery center with the identification of the need or recommendation for surgery. Automating workflow begins with the staff at surgical clinics planning for cases by identifying the prerequisites for surgery and coordinating patient availability and urgency of surgery with facilities that provide services.
Preoperative workups, including consults, tests, and labs, are built into electronic checklists with LiveData PeriOp Planner, where items required to be completed before day-of-surgery admission can be monitored for completion. In order to eliminate the risk of day of surgery cancellations, clinical staff can search for patients whose PreOp Workups are incomplete and follow up with them.
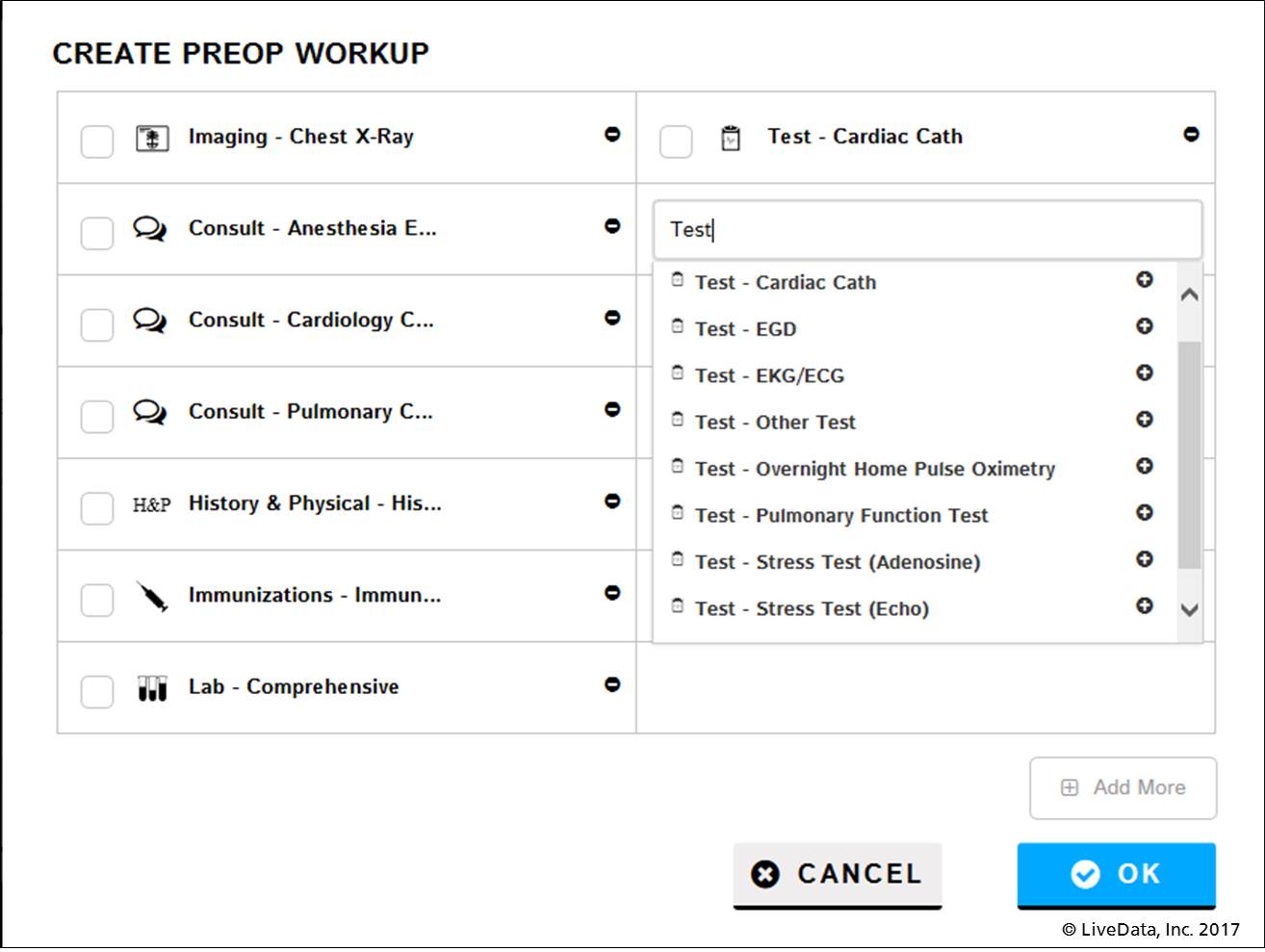
LiveData Surgery Planner PreOp Workup selections for surgical patients. (Image credit: LiveData)
Clinic staff share proposed appointment book schedules of operating room resources, blocks, and cases to coordinate planning and managing operating room schedules with OR managers and schedulers at surgical facilities.
The proposed appointment combined with PreOp Workup checklists allow preoperative clinicians to follow their patients’ progress in preparation for the day of surgery, ensuring timely communication between each healthcare provider, the patient, and the surgical team. Patients and providers are confident in scheduling. No patient preparation step is missed; no operating rooms are left unused.
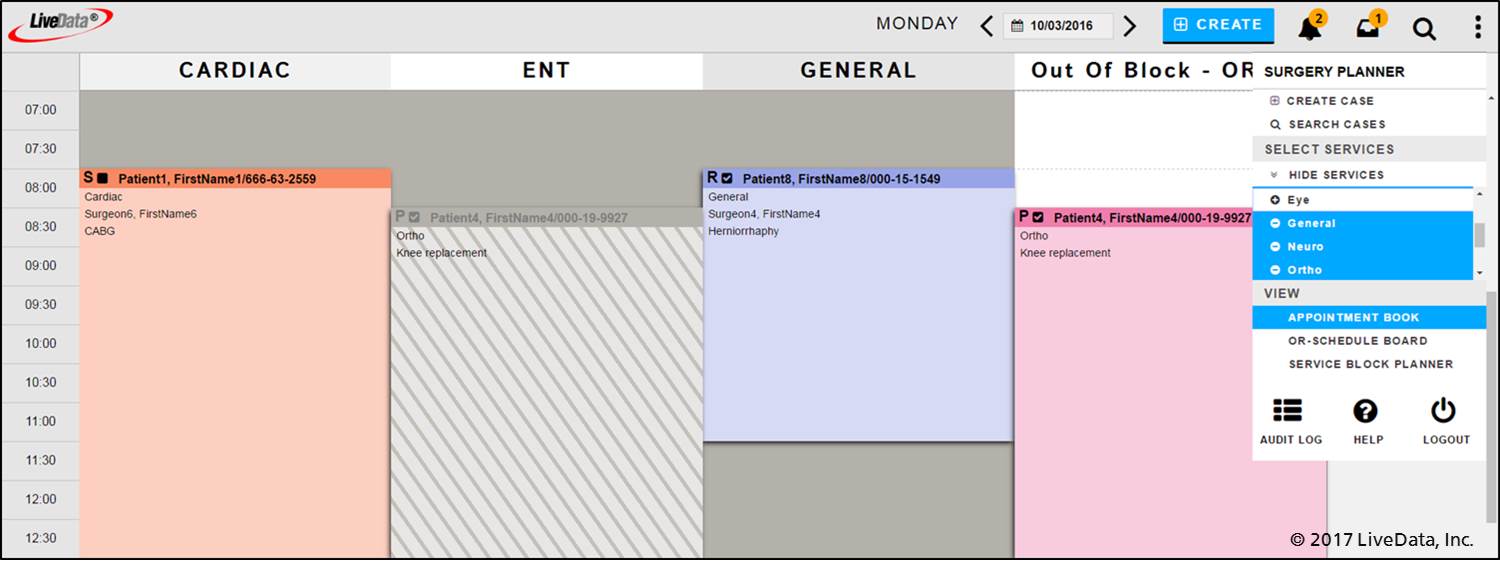
LiveData PeriOp Planner appointment book. (Image credit: LiveData)
Managing the Day of Surgery
When the patent arrives on the day of surgery, he or she is checked into Patient Flow in the hospital. Patient status is displayed on LiveData OR-Schedule Board, a dynamic visual display of the full day’s surgical caseload, and on Family Waiting Board, a display in waiting rooms enabling the patient’s loved ones to follow their progress.
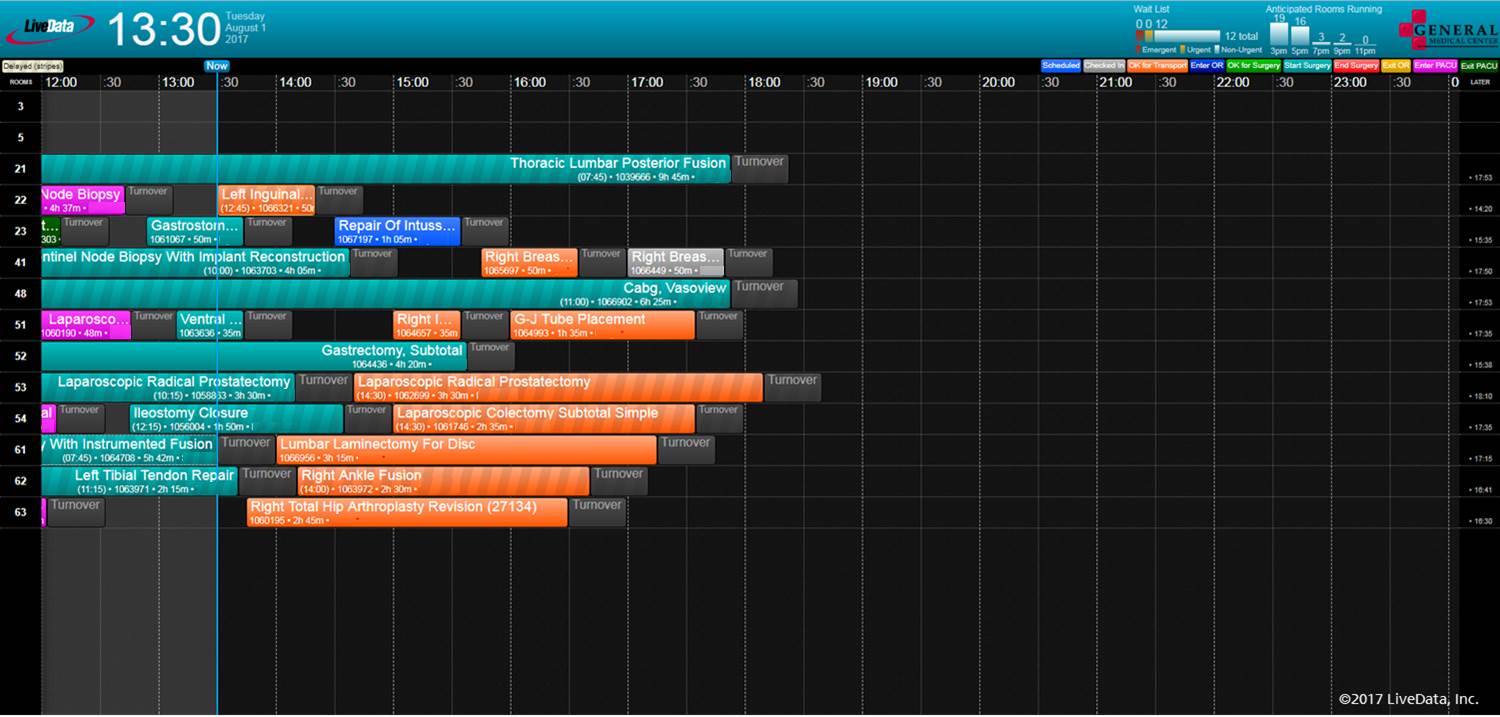
LiveData OR-Schedule Board displays a full-day schedule and case details. (Image credit: LiveData)
Day-of-surgery preoperative milestones are managed on LiveData PreOp Board, an electronic checklist in the preoperative area displaying tests and sign-offs required before entry into an OR or procedure room. Milestones can include completion of history and physical (H&P), consent form, site marking, lab status, blood availability check, EKG, and nurse and anesthesiologist assessment ensuring patient readiness for a move to an assigned OR.
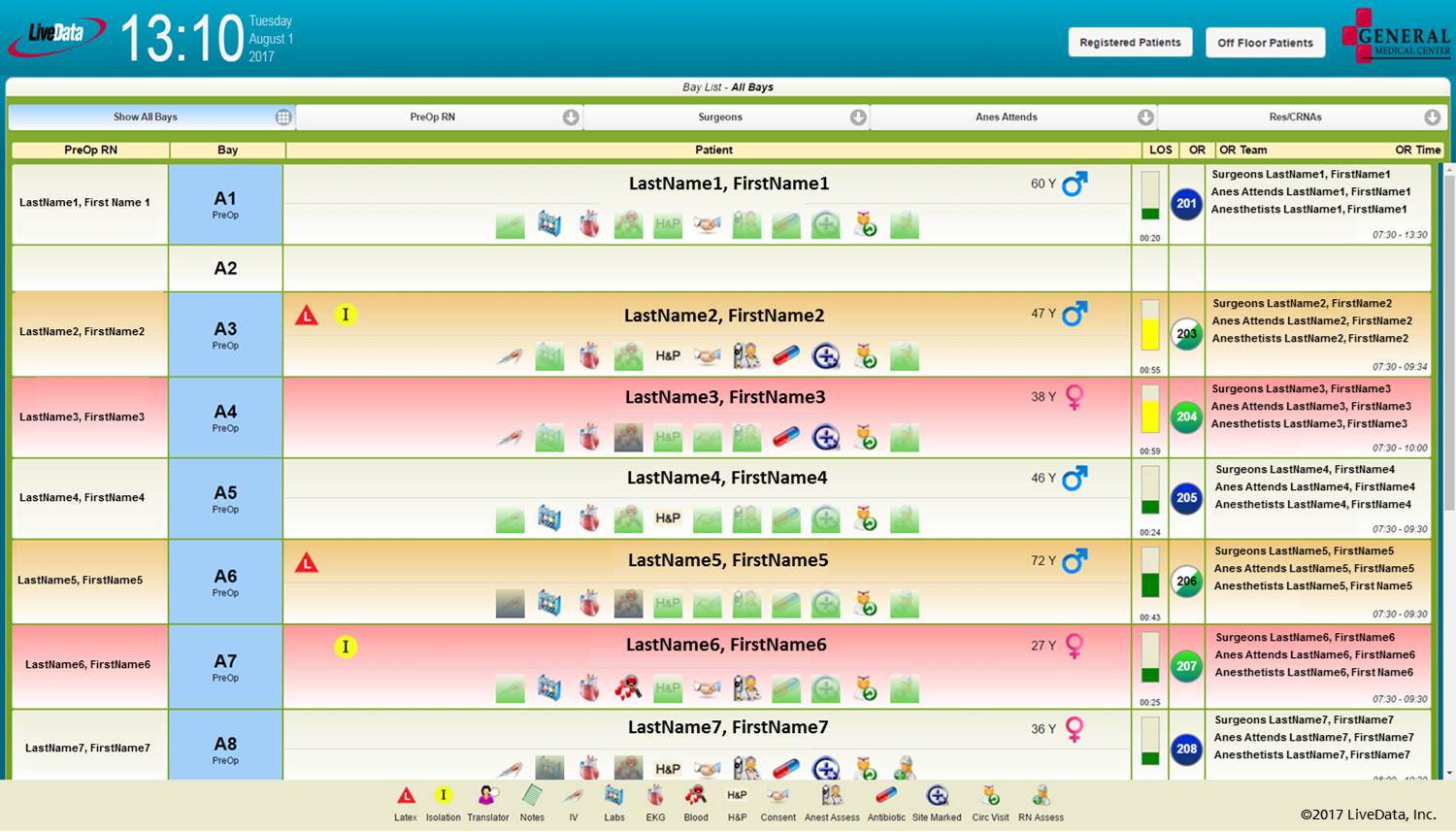
LiveData PreOp Board with day-of-surgery patient preparation. (Image credit: LiveData)
Clinical resources can be managed to make sure each patient and assigned OR are ready at the same time for first case on-time starts and subsequent case on-time starts throughout the day.
Integrating Comprehensive Case Dashboards into the OR
Managing surgical workflow from initial recommendation to day-of-surgery ensures both the patient and facility are prepared: the schedule, times, staff, equipment, and consumables are all in place.
This is confirmed on LiveData OR-Dashboard, which is displayed on a monitor in the assigned OR when the patient enters the room to begin surgery. Patient clinical details from EMR and HIS systems along with data from physiological monitoring devices provide constant updates for the entire surgical team.
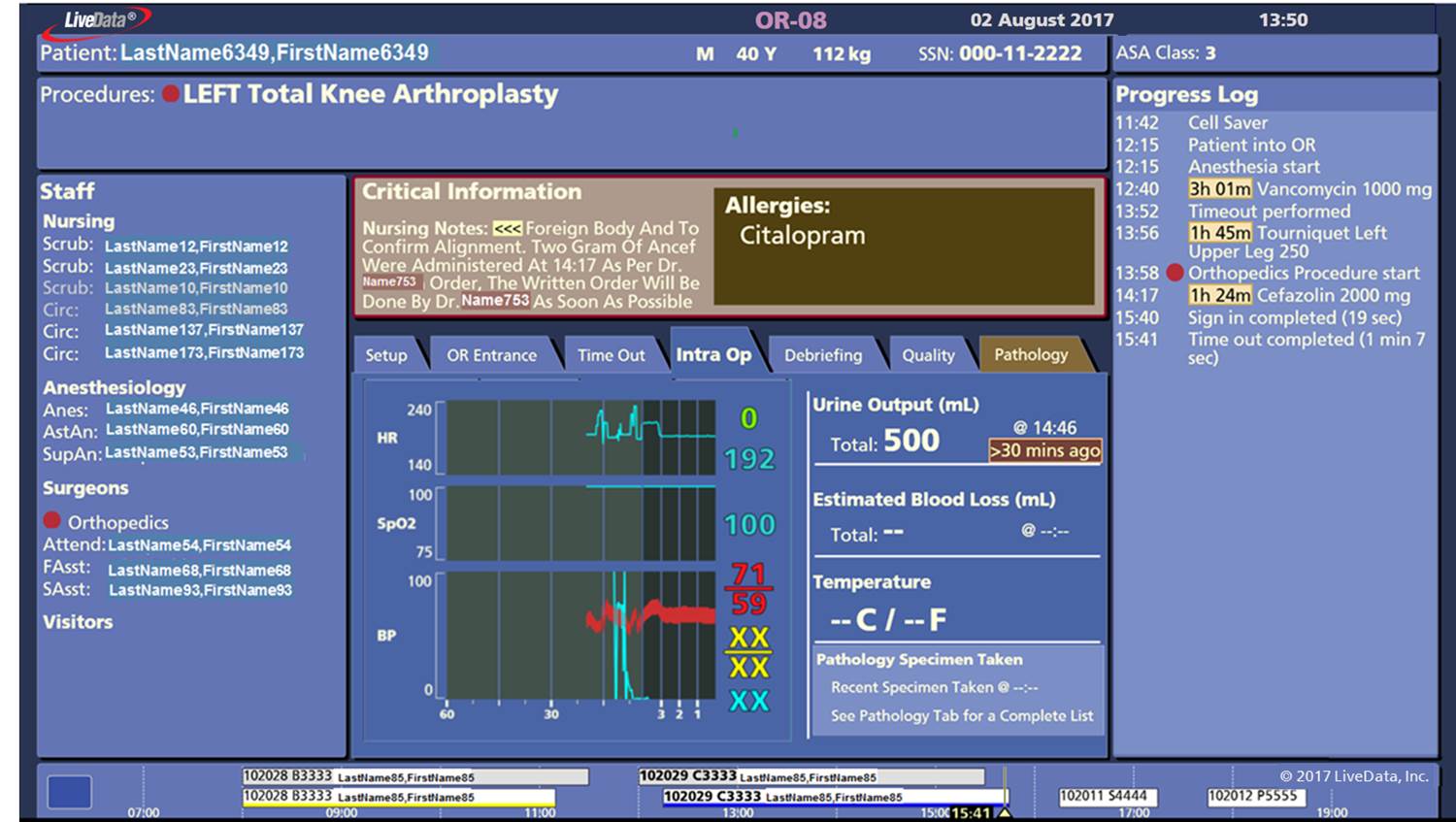
LiveData OR-Dashboard with patient, staff, procedure, physiological monitoring, and progress log. (Image credit: LiveData)
A real-time Progress Log tracks and displays each step of the procedure and workflow, automatically documenting and time stamping the case information. Actual case duration compared to scheduled duration is also tracked and displayed at the bottom of OR-Dashboard.
Meeting Surgical Safety Mandates
Surgical safety checklists are often paper-based tools with a member of the clinical team using the list as a guide to ask questions during the procedure. With OR-Dashboard, checklists can be integrated into the workflow and presented electronically as the surgical team progresses through each step.
LiveData embeds its proprietary Active Time Out (ATO), an electronic safe surgery checklist, into the surgical case workflow. The checklists are recommended by the World Health Organization and mandated as the universal protocol by the Joint Commission. These checklists include Briefing or Pre-induction, Time Out or Pre-incision, and Debriefing or Post-procedure.
Responses using a wireless clicker to step through the questions are automatically captured and documented to ensure each question is answered, time stamped, and documented for compliance reporting.
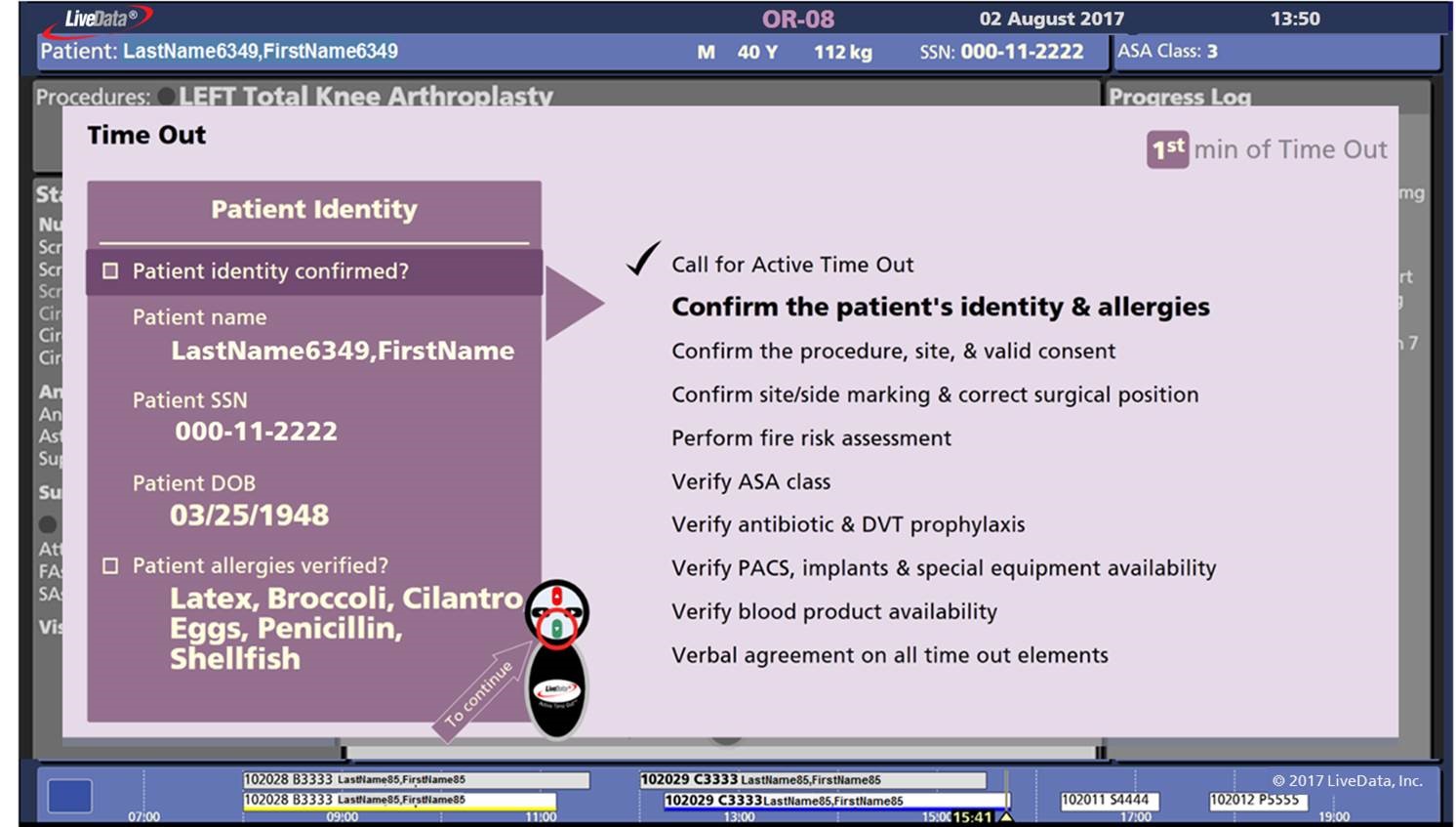
LiveData Active Time Out electronic safe surgery checklist. (Image credit: LiveData)
LiveData PeriOp Manager automatically generates documentation of the case steps with accurate beginning and ending times. The details are integrated into an EMR eliminating manual case documentation. PeriOp Manager communicates this information directly to LiveData PeriOp Manager Analytics, which provides comprehensive analysis of block utilization, checklist compliance, and resource management.
Measuring Workflow Success
Automated workflow enables delivery of coordinated care that incorporates clinical protocols, guidelines for best practices, and perioperative processes. Process standardization supports service operations, performance improvement, and resource management.
Implementing automated workflow across the perioperative environment supports delivering value-based care — consistent, high quality care at the lowest cost. Integrated analytics supports measuring variability, improving outcomes, and sustaining improvements over time.
LiveData PeriOp Manager Analytics transforms the real-time operational data captured from workflow into measurable, actionable quality, compliance, and efficiency intelligence.
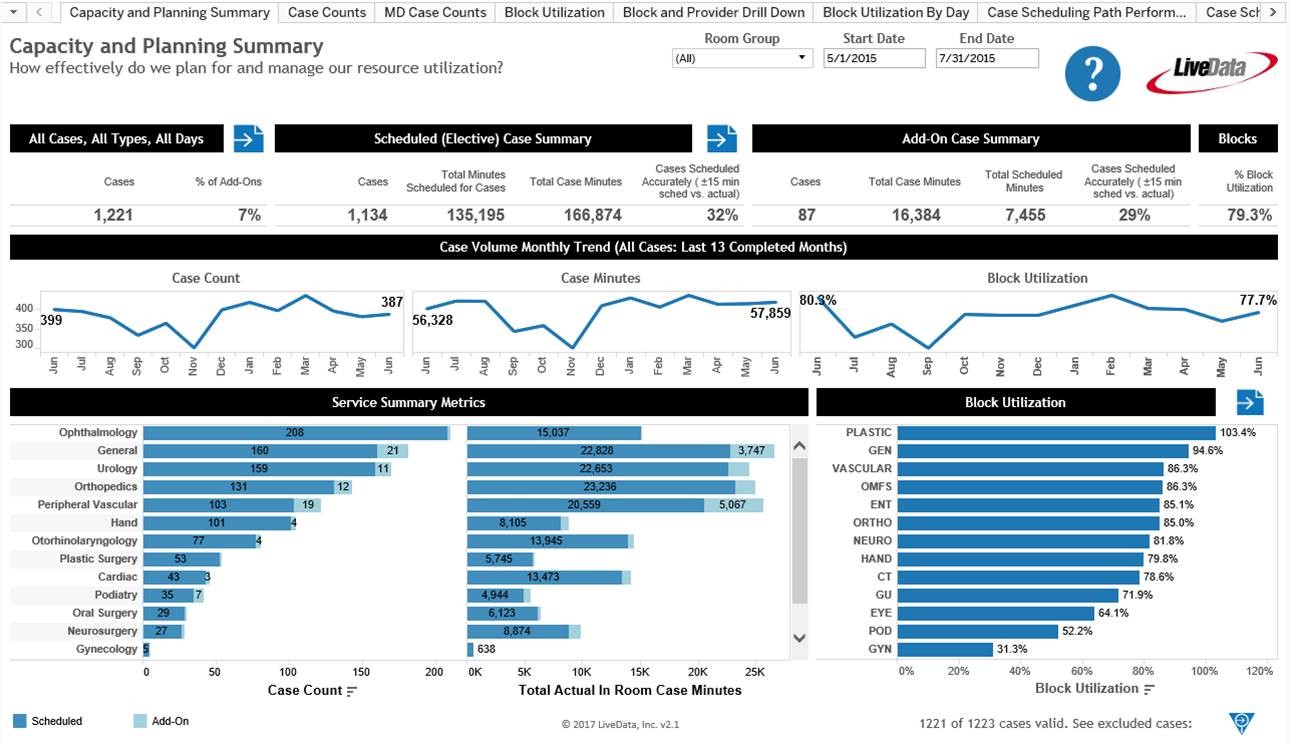
LiveData PeriOp Manager Analytics overview of performance indicators. (Image credit: LiveData)
Data to support achieving key performance indicators is readily available from operational reports including information on surgical capacity and planning, surgical efficiency, and patient safety and clinical quality.
Improving Patient and Provider Satisfaction
With automated workflow informing the surgical journey, patient satisfaction is improved. Each step of the journey is outlined and monitored. Patients and family are guided through surgery preparation and kept informed throughout the process.
Surgical facilities are accurately scheduled and prepared for each patient case to maximize physical and clinical resources. Clinicians can focus on delivering consistent, high quality care at the lowest cost. Hospitals and ambulatory surgical centers can measure and continuously improve services to deliver value-based care.
Jeffrey Robbins has served as strategic and visionary leader of LiveData, Inc. since founding the company in 1991.
This story originally appeared in the September/October 2017 issue of Surgical Products.




